Across the country, primary care networks have started to recruit clinicians and social prescribers through the additional roles reimbursement scheme that provides funding for recruitment to these extra roles. An accompanying blog by Rebecca Rosen and Martin Marshall argues that recruiting to these new roles should be shaped by various local factors.
Many clinicians coming into these posts are working in general practice for the first time, let alone delivering services across networks of practices. Without the support to develop the clinical skills, organisational knowledge and teamwork required, the new roles risk being stressful and wasteful. All of which is made much harder by the social distancing and operational restrictions associated with Covid-19.
This blog examines the practical challenges of introducing these new roles into primary care, and in developing effective multidisciplinary working within GP practices and across networks.
The different parts of inter-professional teamwork
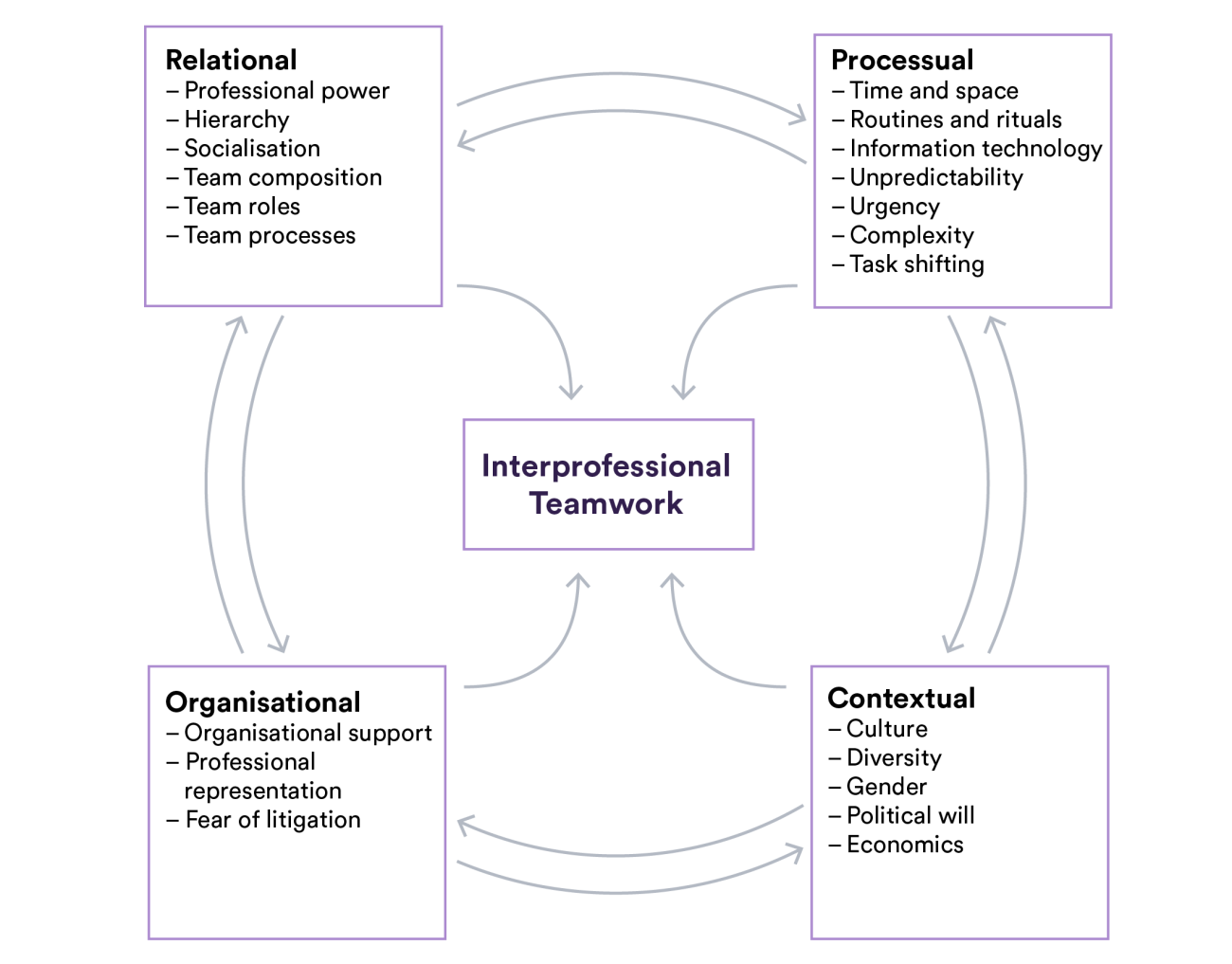
The framework in the image below describes four interlinked components of inter-professional teamwork: relational, processual, organisational and contextual. Using these models as a basis to frame discussions, the participants from our workshop with the RCGP earlier this year highlighted a range of factors that could help practices and primary care networks introduce new roles.
Addressing the practical challenges of implementation
An early challenge for practices and PCNs will be to provide organisational support to facilitate effective interdisciplinary team working. Without this, the introduction of new clinicians to provide care, particularly across multiple practices in a network, is unlikely to be sustainable.
Themes that emerged from the workshop demonstrated the importance of relational and processual factors required for the development of effective interprofessional teams. The two groups of factors are intertwined, as relationships will only emerge and strengthen if the processes are in place to help them do so.
Clarifying the roles and competencies needed for each role is central to determining skill mix requirements at a practice and network level (the importance of which is discussed in the other blog). Role clarity and team composition will be facilitated by having a unified goal and vision, ensuring everyone is working towards a common purpose – in some ways something that Covid-19 has reinforced.
Enabling different team members to work in the same place and the design of workspaces is also important to create opportunities for discussions and help build strong relationships. Considering how and where new staff should work is both a key challenge and a huge opportunity. The way that remote consultations and novel technological solutions have been adopted quickly during Covid-19 may well drive further innovation and creative solutions to the issue of working across multiple sites.
Process factors are important for enabling people to spend time together as a team, to develop a shared identity and to build trusting relationships. The structure of the working day and various digital resources can enable people to step out of their clinical roles to make teams work – to participate in meetings, huddles and other formal and informal methods of communication that are proven to support effective teamwork.
These factors are important to ensure that different professionals are not merely working in silo but in a multidisciplinary way. True multi-professional working also requires a shift in processes, from those which generate top-down solutions for workforce pressures towards more integrated patient-focused care in which team members and patients are encouraged to identify and address problems themselves.
Thinking about teams in this way will impact upon workforce redesign in such a way that, instead of task substitution by one role for another, flexible boundaries between roles allow staff to cover some parts of each other’s work. This flexibility will aid resilience (important in such times) but also, as some work shifts away from GPs, processes must be put in place to safeguard against GPs becoming burdened with an increasingly complex case-mix, yet insufficient time to spend with these patients, and subsequently insufficient time to feed into team building.
Not only is it important for professionals to develop role clarity, shared aims and trust, patients should be actively involved and engaged in the design and implementation of team working from the outset, as an integral part of the multidisciplinary team, ideally through co-design. We should seek to understand patients’ views about seeing different professionals, and also ensure any proposed skill mix fits with individual patient requirements.
Beyond processes and relationships: the need for time
Developing trusting professional relationships and a true understanding of each other’s roles (adapted to context) requires time.
Workshop participants felt that, to a certain extent, trial and error will determine what works well based on the needs of different populations. Overall, there was agreement that there is no ‘off the shelf’ one-size-fits all approach, and that the most needed ingredient is indeed time.
That’s time to develop role clarity, time to build good relationships and trust among both staff and patients, time to allow the team to organically form and adapt to population health and local context, and time to redesign physical space and communications systems.
But given the rapid pace of change required by the specifications within the PCN contract, compounded by the challenges of Covid-19, time is sadly in short supply.
Dr Simona Baracaia is a Public Health Registrar.
Suggested citation
Baracaia S (2020) “Addressing the practical challenges of multidisciplinary teamwork in primary care”, Nuffield Trust comment.