A version of this data blog was first published in the BMJ on 25 January.
Three times as many people were admitted to hospital with flu in the first week of 2018 compared to the same week a year ago, while ambulance handover delays increased and pressure on beds remained high. But are we alone in finding it hard to deal with the pressures of winter? It seems not.
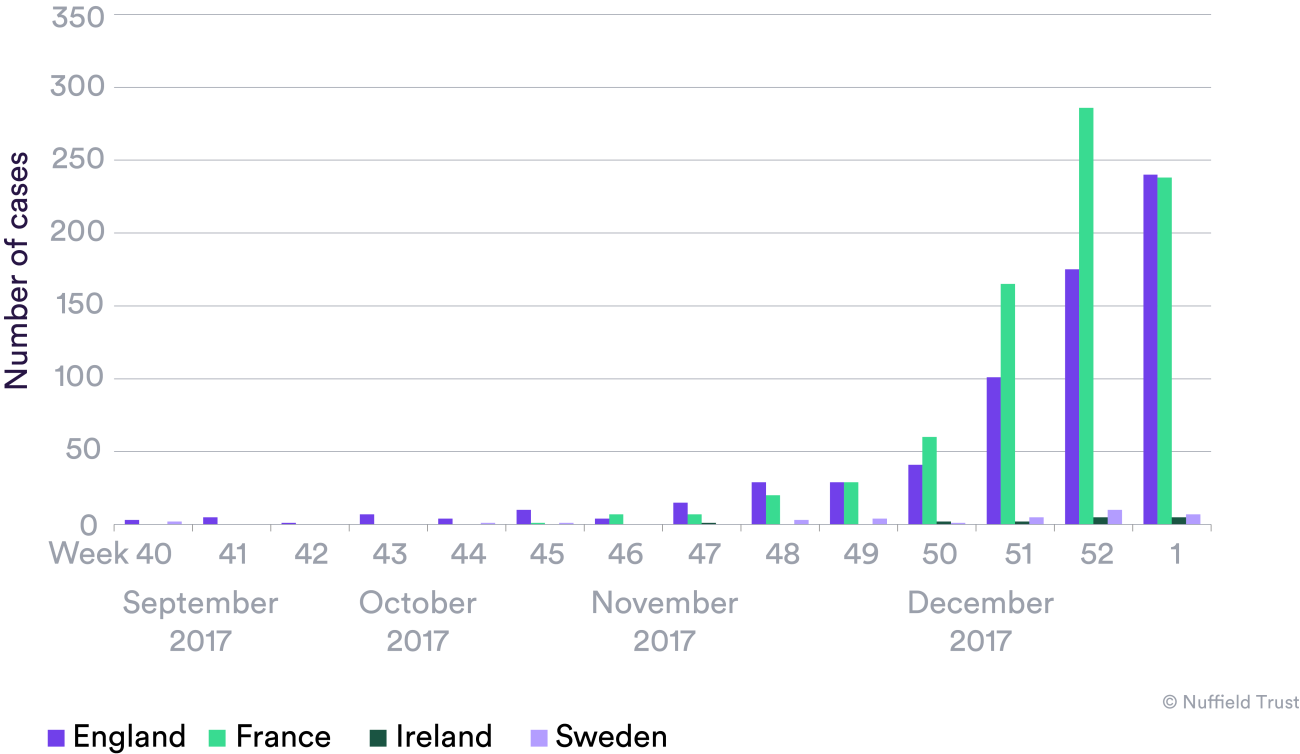
Flu varies across countries, but while the first week of this year saw low numbers of patients admitted to intensive care units in Sweden and Ireland, it was a similar story to the UK in France, where hospital admission rates for flu were also high.
French winter woes
Last winter, the French health minister Marisol Touraine said the country was experiencing an intense flu epidemic, with a total of 142 hospitals on full alert and advised to cancel all non-urgent operations.
This winter, Paris has activated its winter epidemic plan – “deprogramming” non-urgent cases and opening extra beds. Meanwhile in Bordeaux, as demand increases and the hospitals become “saturated”, the advice is: “Go to your GP, not the emergency department!”
Pressures on the French health care service – which in 2016 spent around 8.7% of gross domestic product (GDP) publicly and 2.3% privately, compared with 7.7% and 2% in the UK – are not new. In 2015, a leaked intelligent services memo described the country’s emergency wards as “on the brink of collapse” due to overworked staff and angry patients. A health union leader said the service had become like Britain’s NHS “under Margaret Thatcher”.
Swedish stabsläge
Over in Sweden (which spends 9.2% of GDP publicly and 1.8% privately on health), the Karolinska University Hospital also experienced something of a winter crisis in 2016, with overcrowding after a sharp increase in patients attending its emergency departments.
As a result the hospital went into “stabsläge”, which is essentially a plan to prepare to reallocate hospital resources – such as beds and staff – as well as possibly cancelling non-urgent operations.
In what is perhaps a reflection of a history of higher funding than the UK (and experience of keeping things going even when it snows), no patients in the end had to be moved, although “a small number had to wait nearly 24 hours for a place”.
Irish national emergency?
Meanwhile in Ireland (which spends 5.5% of GDP publicly, 2.3% privately), the head of the Irish Nurses’ and Midwives’ Organisation has called overcrowding in hospitals a “national emergency”.
The health minister, Simon Harris, has said all “the winter plan measures funded by increased investment by government, like increased access to home care, transitional care, and diagnostics along with additional acute bed capacity, are being implemented to deal with the extra pressures our health service is experiencing.”
Winter pressures also hit Australia (which spends 6.5% of GDP publicly and 3.1% privately) back in June. South Australia Health triggered its demand action plan in the middle of the month to deal with a surge in emergency patients – with non-urgent elective surgery being postponed, patients discharged early, and other patients moved to semi-rural hospitals to free up space in major metropolitan hospitals.
What do these countries have in common… and what sets them apart?
The common thread through these global examples is the need that all health services face – seemingly regardless of funding levels – to try and manage spikes in demand for emergency and urgent care.
While funding and organisation differ, strategies are similar. Cancelling non-urgent operations to free up staff and resources, speeding up the rate of discharges, opening extra beds, and allowing waiting times to grow. What perhaps differs is what is seen as a crisis. The problems at the Karolinska University Hospital in 2016 were rare (the first since 2009), and disrupted services for just one morning.
Tough times at home
International comparisons aside, this winter has not only felt tougher for the NHS compared with previous winters, but is demonstrably so.
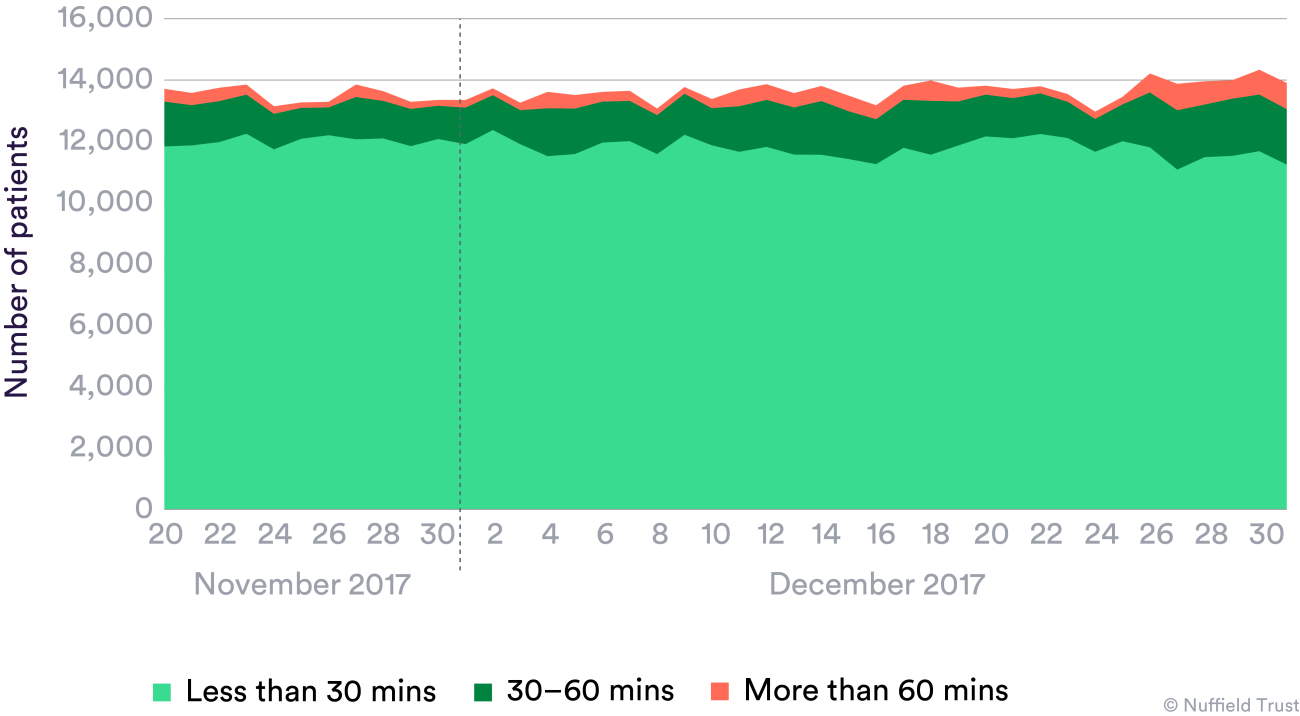
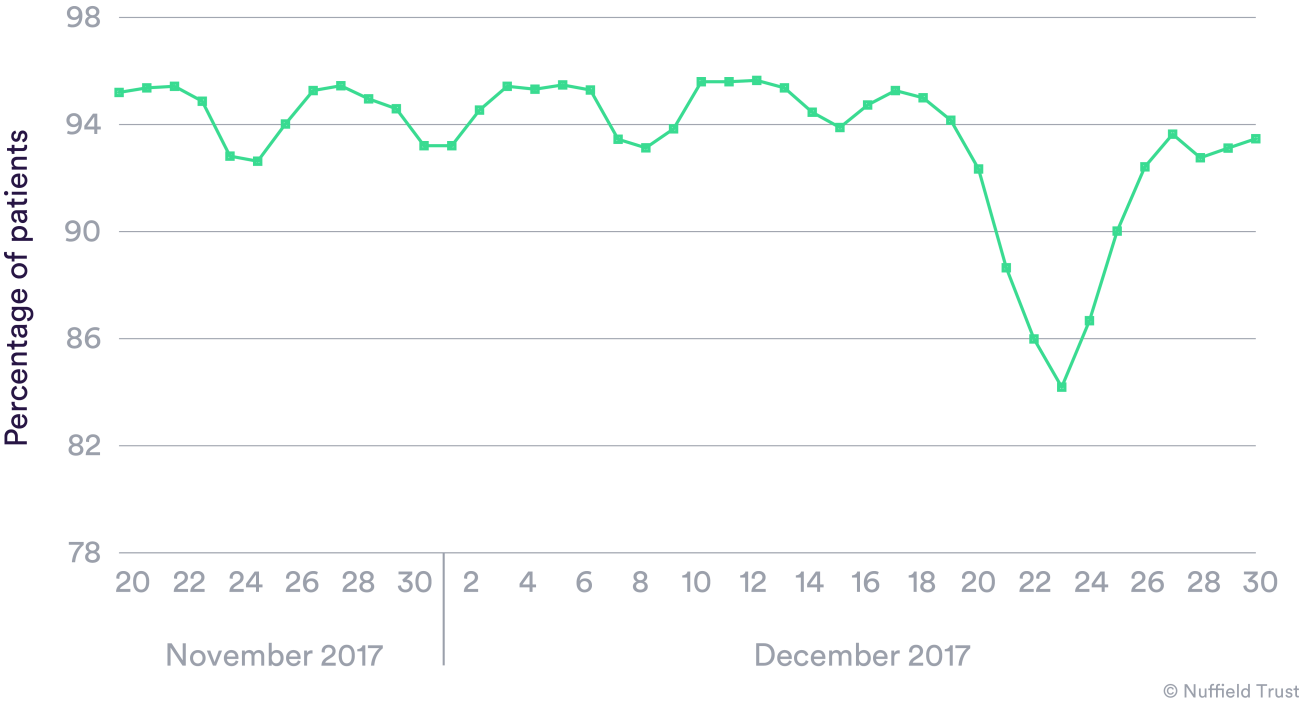
In December, the English NHS had the highest number of attendances at hospital emergency departments, and the highest number of patients waiting over four hours for admission from emergency departments into hospital. It also had the lowest proportion of patients treated, discharged, or admitted from emergency departments within four hours of any December since 2010, with similar pressures in Scotland and Wales.
Update: We know now too that the first month of 2018 was extremely tough on the health service. Over 80,000 patients waited on trolleys for more than four hours at A&E in January, with over 1,000 of those waiting for over 12 hours. These are the highest numbers since records began.
A year since we warned that corridors had become the new emergency wards, it is deeply concerning that the position has since worsened, with many harrowing reports of patients being treated in busy corridors by stressed and overworked staff.
With every part of the health service creaking at the seams, surely by now it is time to face facts and offer sustainable funding increases to the NHS.