Nursing shortages are so severe that the Health Select Committee is currently conducting an inquiry into its causes. Recent figures from NHS Improvement indicate that there are at least 36,000 nursing vacancies in England and the figure could be as high as 42,000.
At the same time, NHS Digital statistics show that the NHS in England is employing 6,000 more nurses than in 2010.
Both things are true.
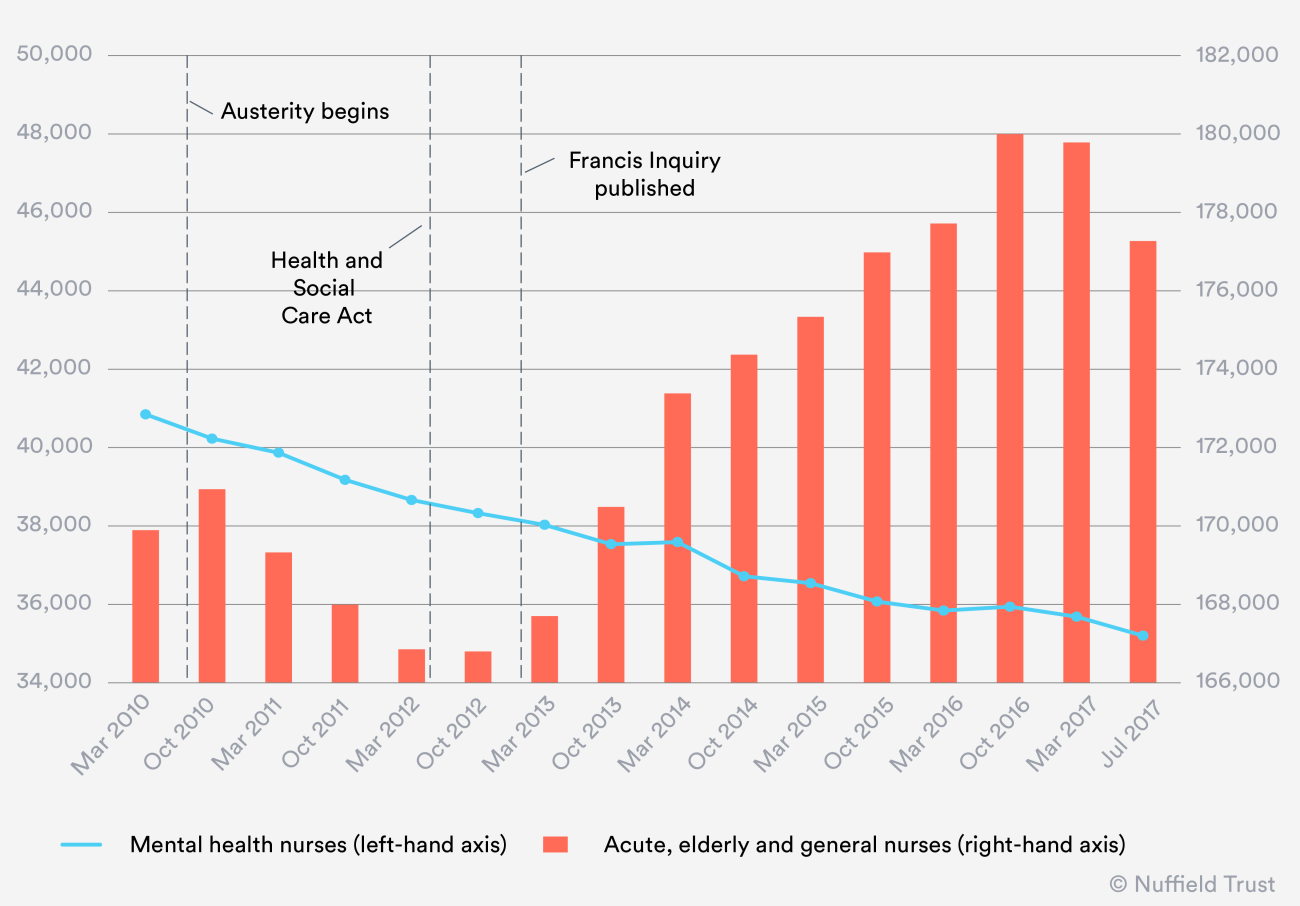
There are more hospital nurses in post than in 2010, yet there are shortages of nurses wherever you look. Each nursing specialty has its problems, but they are not all the same, and as the figure below illustrates, they are not all following the same trajectory.
Why so different?
Turn the clock back to March 2010, a few months before the election that brought the Coalition Government into power. There were 281,983 nurses employed in hospital and community services in England. Within that total, 169,897 were nurses working in acute, elderly and general care – the mainstay of the secondary care sector. Some 40,849 mental health nurses were in post – the high-water mark for this specialty in recent times.
October normally marks the annual high point in nurse employment, and October 2010 was no exception with more than 170,000 acute nurses in post. Fast forward a few months, and the picture begins to change. Austerity has begun. The squeeze on NHS finances means that staffing costs, which account for 70 per cent of hospital expenditure, are an inevitable target for savings.
As nurses form the largest clinical staff group, the drive for cost savings made their posts quite vulnerable. By March 2011, more than 1,600 acute sector nursing posts have gone, and nearly 1,000 mental health nursing posts have been lost.
Parity of disdain?
The trend continues through to March 2012. 4,000 acute nursing posts disappear, along with a further 1,200 mental health posts – more than one in twenty. In April of the same year, the Health and Social Care Act puts mental health on an equal statutory footing with physical health. Parity of esteem is the new buzzword.
As far as nursing posts are concerned, parity of disdain might be a better description. Nursing posts continue to be whittled away. Another 1,800 acute nursing posts disappear over the next six months, reaching a low point of 165,000 nurses for acutely ill and elderly patients. By this point there are 2,714 fewer psychiatric nurses employed – a drop of 6.6 per cent.
Divergent paths
In February 2013, the Francis Inquiry report is published, and the impact on nursing employment is immediate. Within a month, the number of nurses caring for adult patients rises by 200, by a further 450 the following month, and by October 2013 numbers have risen by more than 2,000. Growth continues month on month until May of this year.
The trend is downward again now, not because posts have been cut but because vacancies cannot be filled. It is the top cause of worry for most chief executives according to NHS Providers.
The trend in mental health nursing numbers has held steady. Sadly, that trend is downwards. NHS Digital figures show a relentless attrition of several hundred posts month after month after month. Vacancy levels are now at 10 per cent. The CQC signalled serious concern in July. The Department of Health responded with an ambitious plan to increase mental health capacity, improve services and end out-of-area treatments. None of these aims can be met unless existing vacancies can be filled, making the job less stressful, more doable and more rewarding.
Understanding these trends
The trajectories for mental health and acute nursing may look rather different, but of course there are some shared factors in play. Just because acute nursing numbers recovered from their low point in September 2012 and are now 7,000 higher than in 2010 doesn’t mean there were enough nurses in post either back then or now. Patient acuity and inpatient activity have both increased far faster than nursing numbers. Length of stay has shortened, increasing the pressure on nurses whose patients are sicker during their spell in hospital.
March 2009 saw the highest number of mental health nurses in post in the last decade. But is that an appropriate baseline? Excessive caseloads for community psychiatric nurses and hand-to-mouth staffing in mental health settings are not a new phenomenon.
And getting an accurate picture of how and where mental health workers are deployed is so complex that the UK Statistics Authority has asked NHS Digital to consider further work in this area.
And the stark fact remains that we had fewer mental health nurses in post during 2017 than in 2000.
The spirit of the law?
Nurse workforce planning has been so woefully inadequate for so long, that it barely deserves the name. It took an eminent QC, Sir Robert Francis, to force the acute sector to change tack and to recognise that patient safety, wellbeing and recovery depend on having sufficient skilled nurses in post. 5,000 posts were lost before the NHS secondary care sector came to its senses and started recruiting for safety and quality.
Another QC, Sir James Munby, has blown the whistle on gaps in mental health provision for vulnerable young people, describing it as “utterly shaming” that no bed could be found for a vulnerable teenager without judicial intervention.
A workforce plan for the whole NHS has just been published for consultation. We have to hope that the mounting chorus of concern helps ensure that plans to improve mental health staffing move swiftly from aspiration to reality.
That would be parity of esteem at last.