Over a year and a half into the Covid-19 pandemic, we have become familiar with daily data on the numbers of new cases, hospital admissions and deaths, and during 2021 the more welcome numbers of people vaccinated.
While the respective health services across the UK have faced many similar challenges during this period, UK-wide reporting has masked any differences in peaks and troughs across the four countries. This reflects how Covid-19 has spread over time, and the impact of new strains of the virus and lockdown rules, among other factors.
In this explainer, we take a closer look at the pandemic across the UK to date, including where some of those differences have been between each country, while also describing the shared challenges and implications for health services across the UK in the coming months.
From the first wave to the third: how have case numbers changed?
In the first wave of the pandemic, from March to May 2020, limited testing was available, particularly out of hospital, so numbers of confirmed cases vastly underestimated the actual number of infections. Even Covid-19 deaths and hospital admissions were also under-reported.
Confirmed cases became a more useful way to track variation across the four countries when widespread testing was rolled out towards the end of May last year. It’s still worth noting that variation in testing capacity and roll-out of testing programmes, such as testing in schools, impacts on the numbers of cases identified.
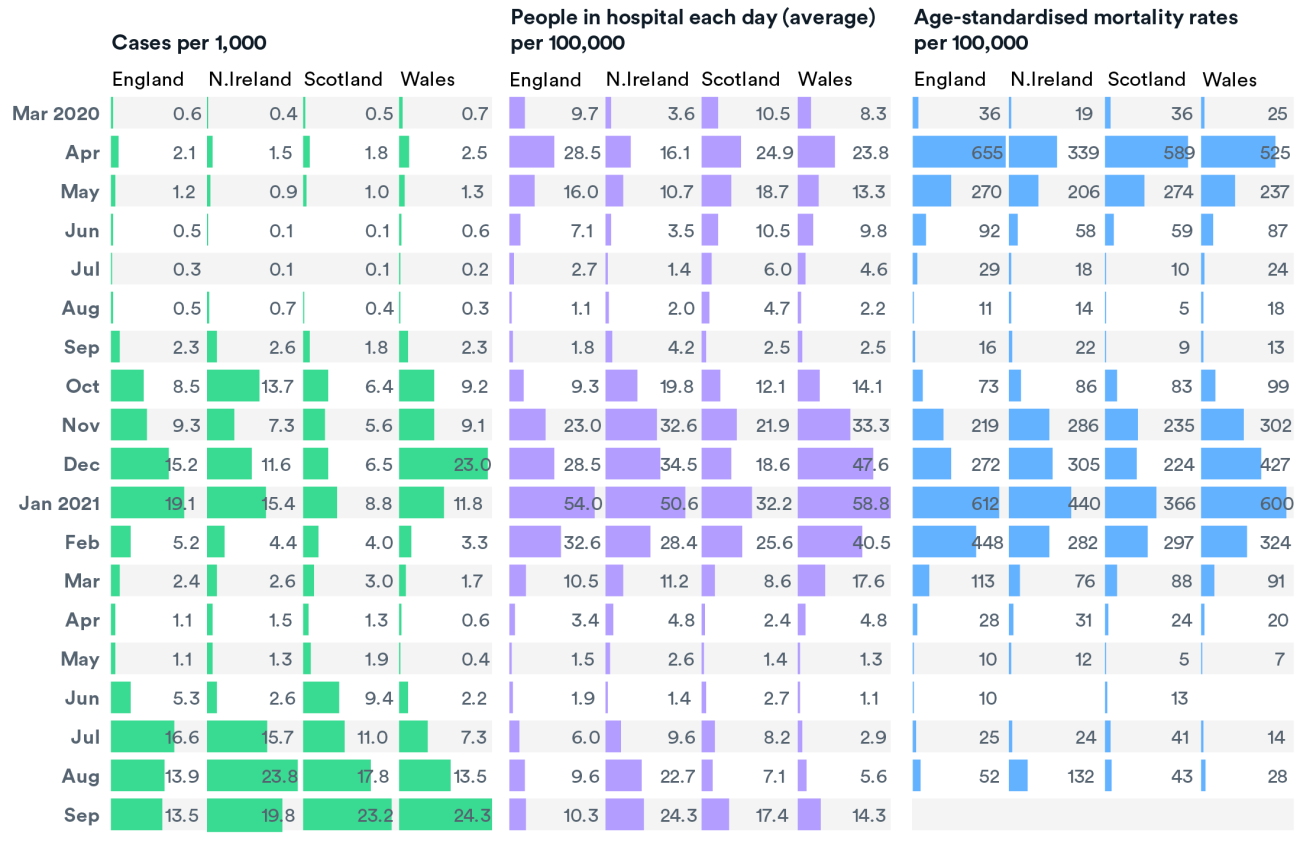
In the second wave, from October 2020 to February 2021, cases in Northern Ireland started to increase earlier in the autumn, but were contained by a series of lockdown measures introduced from the end of September onwards. Infection rates increased in England from October, stalling during the lockdown in November, but then increased rapidly as the “Kent” variant (later also called Alpha) took hold, peaking in January.
Cases also increased quickly in Wales, peaking in December. Wales initially introduced a short firebreak in October, which was followed by further restrictions in early December. Scotland was able to keep case rates, hospital admissions and deaths at lower levels than the other UK countries during this period, probably reflecting a combination of earlier lockdown in October and the slower spread of the “Kent” variant north of the border.
The third wave, since July, has again been widespread across the UK, driven by the much more contagious Delta variant, which became dominant in the UK from the end of May onwards.
The spread of Covid in the third wave has been complex to track, with differences in the demographic profile of cases, and higher case rates occurring in areas that had previously fared relatively well. In part this is likely to reflect the level of immunity following vaccination and previous infection rates. The vaccination programme started last December, with health and care workers, care home residents and people over 80 receiving their first jabs.
There have also been differences in behaviour and social mixing in the third wave. Whereas the first and second waves were controlled by lockdowns, the third wave has been accompanied by reductions in control measures, albeit at different speeds across the UK. The occupational and household factors that resulted in high rates of Covid in the first and second waves are less apparent in this wave. Instead, social factors associated with higher rates of mixing appear to have been more important in recent months.
A case in point is the very sharp rise in cases that Scotland and England experienced in July, coinciding with lockdown rules relaxing at the same time that British football teams competed in this summer’s Euro 2020 competition. The level of football-related cases is apparent in the earlier peak in Scottish cases, which dropped off after Scotland were knocked out of the competition on 22 June. In England, nearly 10,000 cases have been directly linked to spectators attending matches at Wembley, but this almost certainly underestimates the full impact arising from large numbers of people gathering in pubs, bars and private homes to watch matches during the tournament.
In late August, cases increased significantly in Scotland, reflecting social mixing as children returned to school and more people travelled to work outside the home. This peaked on 6 September. Wales has also seen a surge in cases following the reopening of schools in September, which is now declining.
In contrast, cases in England oscillated at an average of about 25,000 per day during September. While cases in school-age children increased, this was accompanied by a decline in cases in the 20-29 age group. Part of the explanation may be that higher levels of cases in England in previous waves and earlier this summer have provided sufficiently higher levels of immunity to prevent a surge in cases when schools returned.
How has the impact of rising Covid-19 cases on hospital services changed over time?
Comparing the numbers of people in hospital and deaths from Covid across the pandemic (see the next chart), it is clear that the second wave was the most deadly in all four countries, with high rates of Covid deaths from November to February. Deaths peaked on 19 January, when 1,484 Covid deaths occurred across the UK. (1,820 deaths were reported on Wednesday 20 January, including a number of cases that occurred over the previous weekend.)
The numbers of Covid patients in hospital were high over a period of many months between November and February. On 18 January, there were 39,254 Covid patients in hospital, occupying about 30% of all NHS hospital beds in the UK.
In the third wave, while the numbers of people admitted to hospital have followed the same trends as cases, the scale of increase is much reduced.
The high vaccination rate in all four UK countries means that even though cases this summer reached similar levels to the second wave – or higher in Scotland and Northern Ireland – the numbers of patients in hospital have not risen to the same extent, as far fewer people go on to develop severe disease. Public Health England estimated that the vaccination programme had directly averted over 82,100 hospitalisations up to 8 August this year. And taking account of reduced transmission due to vaccination as well as the protection of people who have been vaccinated, they estimated that vaccines prevented between 102,500 and 109,500 deaths up to 20 August this year.
While hospitalisations and deaths broadly follow case rates in all four countries, Northern Ireland appears to have higher rates of hospitalisation in the third wave, relative to numbers of cases. In the latest wave, the rates of people in hospital with Covid have also been highest in Northern Ireland, with an average of over 24/100,000 people in hospital in September, compared with 10/100,000 in England, 17/100,000 in Scotland and 14/100,000 in Wales. Deaths have also been highest in Northern Ireland in this wave, with 132/100,000 during August, compared with 52/100,000 in England, 43/100,000 in Scotland and 28/100,000 in Wales.
It is unclear at this point why Northern Ireland has experienced higher hospitalisations and deaths in this wave. Possible explanations could be marginally lower vaccination rates in Northern Ireland, relatively worse underlying health conditions, or differences in how health services are treating Covid.
The vaccination programme has enabled almost all restrictions to be lifted across the UK, although more remain in Northern Ireland, despite continuing high case rates. However, Covid is still resulting in significant pressure on health services. It’s worth pointing out that when the England lockdown was announced on 31 October last year, there were 1,240 new Covid admissions, equivalent to 2.2 admissions/100,000 people. This level has already been exceeded in Scotland, Northern Ireland and Wales in this wave, despite the protective effect of vaccinations on severe disease.
Furthermore, there are other pressures on health services, in addition to Covid, which may mean that renewed social restrictions may still yet be required.
In previous waves when lockdowns were imposed, visits to A&E and other health services plummeted. This resulted from a combination of patients choosing to stay away due to anxiety about contracting Covid or concern about putting pressure on the NHS, and reduced demand, as rates of other infections and injuries reduced.
The situation is very different now – with demand for urgent care returning to or exceeding pre-pandemic levels, resulting in the return of long waits for patients in A&E across the UK. Reports from Scotland and Wales highlight the extent of pressure that the service is under.
What are the implications for health services for the coming winter?
As we approach the second winter of the Covid-19 crisis, the shape of the pandemic in terms of the number and nature of cases is unclear, as is the relationship between cases and pressure on care services. Some factors are reasons for optimism, others are not.
The numbers of people vaccinated are continuing to increase, with children aged 12-15 also eligible for a single dose. Vaccinations in younger age groups will reduce transmission, but it will have a marginal impact on the numbers of people with severe Covid who require hospital care. The booster programme for people over 50 is now being rolled out to ensure high rates of protection from severe disease in people most likely to become severely ill or die.
As well as the vaccine programme, we now have an expanding range of treatments for Covid, from extended monitoring for people at home, to new drugs, including for people who do not have an antibody response.
But even though the NHS has developed a much more comprehensive response to Covid, it is also working to recover other services. This includes a backlog of people needing planned treatment, and a surge in demand for emergency care. While the NHS maintained more elective activity in wave two than wave one, it was helped by a drop in demand for urgent care. There is no sign so far that demand on the NHS is reducing during the latest wave, and continued high numbers of Covid cases and hospitalisations are likely to make it impossible to fully recover planned services, let alone increase capacity to address the backlog of people waiting.
This pressure on services needs to be seen against a backdrop of the intense workload for health and care staff over the last 18 months. The long-term impact of fatigue among NHS and social care workers on staff sickness and turnover is unclear.
And then there are significant areas of uncertainty, including the extent of flu this winter, inherent uncertainty about future Covid variants, and how the population responds to the ongoing threat of the virus. The impact of social gathering for the Euros demonstrates the extent to which behaviour drives the pattern of Covid transmission. This is a major area of uncertainty for modelling the spread of the disease, but also indicates that the severity of future waves could be mitigated by influencing social mixing.
The government winter plan sets out the data that will be monitored to ensure that the NHS does not come under unsustainable pressure. The measures of Covid-19 spread include key ones such as the rate of growth in cases in people over 65, while the measures of pressure on the NHS are focused on hospital and ICU occupancy. However, given the pressure already on the NHS, it’s not clear what the trigger will be for introducing any new Covid measures in the coming months.
Covid rates across the UK remain extremely high relative to other European countries, and while there are variations between countries, we are likely to see NHS services across the UK stretched further this winter.
Suggested citation
Scobie S (2021) “What has been the impact of Covid-19 across the UK countries?”, Nuffield Trust explainer.