Since 1983, NatCen Social Research’s British Social Attitudes (BSA) survey has asked members of the public in England, Scotland and Wales about their views on health and care services. The latest survey was carried out between July and October 2019 and asked a nationally representative sample of 3,224 people about their satisfaction with the NHS overall, and 1,075 people about their satisfaction with specific NHS and social care services. The 2019 BSA survey questions reported here were jointly sponsored by the Nuffield Trust and The King’s Fund.
We publish at a time of unprecedented crisis for health services, the economy and society in the form of the COVID-19 pandemic. It is important to bear in mind that the timing of the survey itself means the results reflect attitudes before the emergence of the novel coronavirus. How this pandemic unfolds over the coming months and the way the NHS and care organisations respond are important factors that are likely to influence results from future BSA surveys.
The BSA is a ‘gold standard’ survey that uses a robust methodology to explore public views. The methodology is based on a randomly selected sample of the British public, and is conducted via a face-to-face interview, with multiple follow-up requests to non-responders. The survey is conducted the same way every year, with some topics and questions changing from year to year. The results provide a rich time trend, adding a depth and context to the findings that no other measure of NHS satisfaction provides.
Key findings
Satisfaction with the NHS overall in 2019
- After falling for the last two years, public satisfaction with the NHS overall rose significantly in 2019. Overall satisfaction was 60% – a 7 percentage point increase from the previous year.
- Older people were more satisfied than younger people: 68% of those aged 65 and over were satisfied with the NHS compared to 58% of those aged 18–64.
- While satisfaction was highest among supporters of the Conservative party (at 68%, a 10 percentage point increase compared to 2018), there were significant rises in satisfaction across supporters of all the main political parties (Liberal Democrats, 60%, a 10 percentage point increase; Labour, 57%, a 6 percentage point increase).
- The top reason people gave for being satisfied with the NHS overall was the quality of NHS care (68%), followed by the fact that the NHS is free at the point of use (60%) and that it has a good range of services (49%).
- The main reason people gave for being dissatisfied with the NHS overall was staff shortages (62% – an increase of 10 percentage points since 2018), followed by waiting times for GP and hospital appointments (57%), and a view that the government doesn’t spend enough money on the NHS (49%).
- More people thought that the general standard of care provided by the NHS would get worse (42%) rather than better (29%) over the next five years. This is an improvement on the 2018 survey, where the majority of people (51%) expected care to get worse.
Satisfaction with specific NHS and social care services in 2019
- Satisfaction with GP services was 68% in 2019 – a 5 percentage point increase on the previous year, taking satisfaction with GP services back to just below the level it was in 2015.
- There was little change in satisfaction with inpatient (64%) and outpatient services (71%). Outpatients continue to be the highest-rated service in the survey.
- There was also little change in satisfaction with accident and emergency (A&E) and NHS dentistry services. A&E remains the NHS service respondents are least satisfied with.
- There was little change in satisfaction with social care services, which remains low at 29%.
- People who had used or had contact with individual NHS and social care services in the last year were more likely to express a view about their satisfaction or dissatisfaction with services than non-users, with both satisfaction and dissatisfaction being higher among users compared to non-users.
Funding for the NHS
- As in the previous years, in 2019 most survey respondents (80%) said that the NHS is facing a major or severe funding problem. However, this figure has fallen 6% over the last two years (down from 86% in 2017).
- The majority (54%) of people surveyed would prefer extra funding for the NHS to come from taxation, as opposed to, for example, increased patient charges.
How satisfied is the British public with the NHS overall?
As we enter a new decade, the NHS is facing significant levels of pressure and remains a top concern for the public (Ipsos MORI, 2019). Workforce shortages are affecting patient care and staff experience (Beech and others, 2019).
A&E waiting times are the worst they have been since current records began – a sign of a system that is struggling to keep up with demand (Morris and Davies, 2020). Key targets are regularly being missed and we are performing less well than similar countries on some of the biggest causes of death, including cancer, heart attacks and stroke (Dayan and others, 2018).
Nevertheless, the NHS continues to treat increasing numbers of patients, remains free at the point of use and, over the last two years, has been promised an increase in funding. Notably, in June 2018, the then Prime Minister Theresa May announced that the NHS in England would be given an extra £20 billion a year by 2023/24, with proportionate increases in other regions of the UK.
In 2019, the fieldwork period for this British Social Attitudes survey began in the same month that a new Prime Minister took office. In the months that followed, the extra funding for the NHS which commenced in April 2019 was confirmed and promises were made for extra capital and hospital buildings. A general election was called at the end of the BSA survey fieldwork period.
So what impact has all this had on the public’s overall satisfaction with the NHS? Is it possible that the new funding announcements will lead to improved satisfaction with the NHS, or will evidence of staff under pressure and continuing long waiting times see the recent declines in overall satisfaction continue?
Methodology
The 2019 survey consisted of 3,224 interviews with a representative sample of adults in England, Scotland and Wales. Addresses were selected at random and visited by one of NatCen Social Research’s interviewers. After randomly selecting one adult (aged 18 or over) at the address, the interviewer carried out an hour-long interview. The participant answered most questions by selecting an answer from a set of cards.
The sample size for the overall NHS satisfaction question was 3,224 in 2019. For questions about satisfaction with specific NHS and social care services, the sample size was 1,075. The data is weighted to correct for the unequal probabilities of selection, and for biases caused by differential non-response.
The weighted sample was calibrated to match the population in terms of age, sex and region. The margin of error in 2019 for the health questions was around +/- 1.5 to 3.7 percentage points.
The vast majority of fieldwork for the survey was conducted between July and October 2019.
Topics
The topics covered by the survey change from year to year, depending on the identities and interests of its funders. Some questions are asked every year, some are asked every couple of years, and others are asked less frequently.
Funding
The survey is funded by a range of charitable and government sources, which change from year to year. The survey is led by NatCen Social Research. NatCen carries out research in the fields of social and public policy.
Overall satisfaction with the NHS in 2019
For 37 years, the BSA survey has asked a sample of the public how satisfied or dissatisfied they are with the way in which the National Health Service runs nowadays.
In 2019, 60% of the public were ‘very’ or ‘quite’ satisfied with the NHS (Figure 1). This 7 percentage point increase over the previous year is statistically significant.
Public dissatisfaction with the NHS was 25% in 2019, down from 30% in 2018. This fall was also statistically significant and is the lowest level of dissatisfaction reported since 2017.
This data gives its richest insights when viewed over decades rather than years. Taking that long-term view, Figure 1 shows that the 2000s were characterised by increasing satisfaction, up by 28 percentage points over the decade – from 42% in 2000 to 70% in 2010. The 2010s started with a steep drop in overall satisfaction (from 70% in 2010 to 58% in 2011). Since then, levels of satisfaction have ebbed and flowed. However, falls in satisfaction in 2017 and 2018 were reversed in 2019.
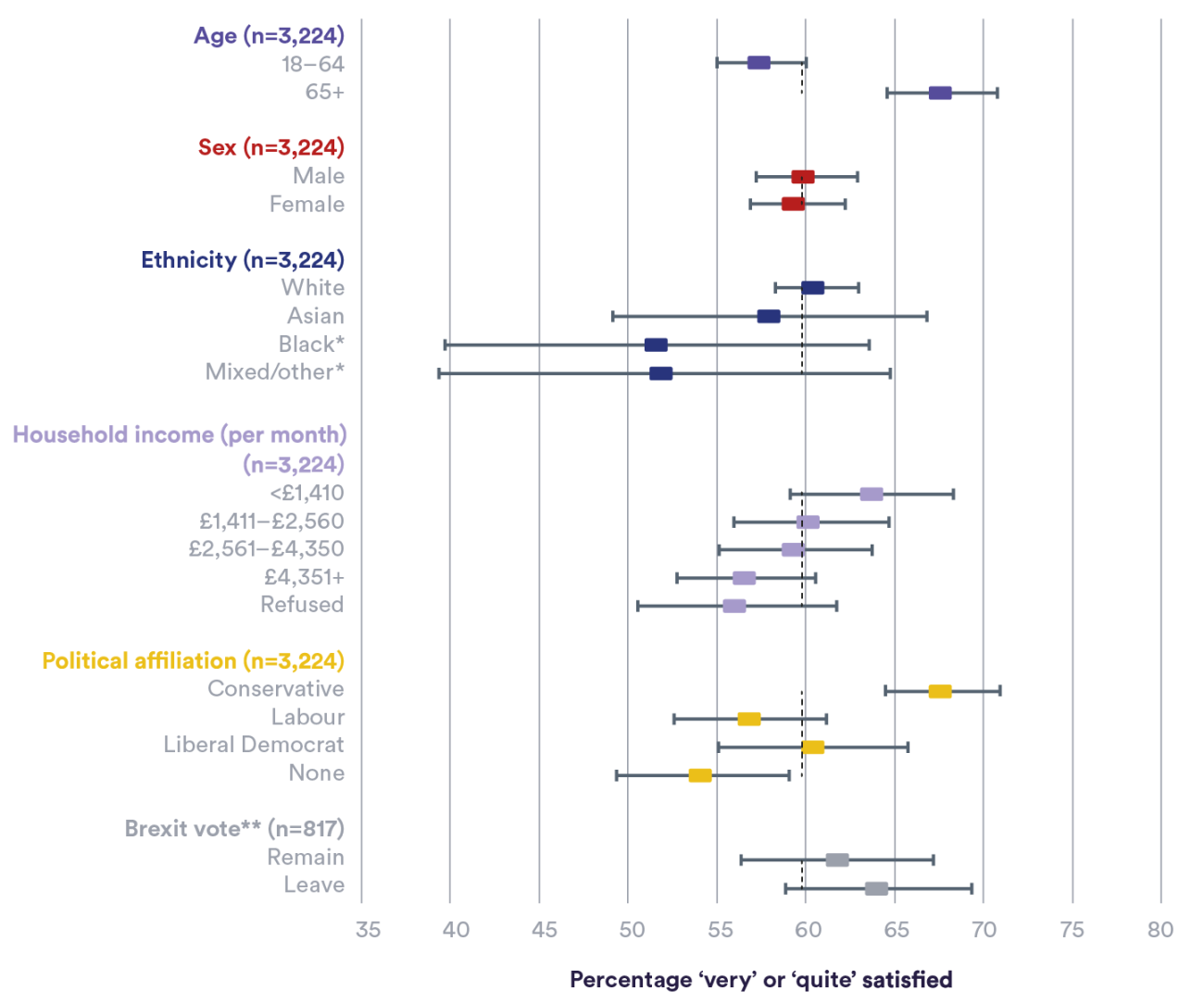
Who is most satisfied with the NHS? Looking below the headline figures on satisfaction with the NHS reveals a varied picture depending on, for example, respondents’ age, party political affiliation and sex. Figure 2 shows how satisfaction differs among different population groups and whether satisfaction is statistically different from the average for the whole survey, which is 60%. As in previous years, satisfaction levels differ by age: respondents aged 65 and older have higher levels of satisfaction (68%) than those aged 18–64 (58%).
While other groups also show differences in satisfaction levels relative to each other, except for party political affiliation these differences are not statistically significant (the 95% confidence intervals overlap) and are generally no different from the average for the whole survey.
Figure 2 also shows that while there are interesting gradients in satisfaction within some groups – for example, lower-income households tend to be more satisfied than higher-income households and White and Asian respondents tend to be more satisfied than Black and other minority ethnic groups – these differences are not large enough given the size of the sample to reach statistical significance, although the pattern is similar to previous years.
There are also differences in the satisfaction levels reported by supporters of political parties. Respondents who support the Conservative party have a higher level of satisfaction (68%) than respondents who support the Labour party (57%) (Figure 2). This follows a pattern seen in the BSA survey in most years, with supporters of the political party in power generally reporting higher levels of satisfaction than supporters of the main opposition party (Figure 3). It is noteworthy, though, that between 2018 and 2019 satisfaction increased significantly across supporters of all main political parties (Conservative, Labour, Liberal Democrats).
While there has been a significant increase in satisfaction across the whole BSA sample between 2018 and 2019, is this reflected across different sub- groups in the survey?
While satisfaction levels have indeed increased across almost all groups, not all of these changes were statistically significant (i.e. it is possible that the changes in the 2019 data were due to chance) (Figure 4). Statistically significant changes in satisfaction were found for people aged 18 to 64 (increasing from 51% in 2018 to 58% in 2019), men (from 53% to 60%), and women (from 54% to 60%). Satisfaction among White respondents increased from 54% to 61%, and satisfaction increased across all main political parties (Conservatives, 58% to 68%; Liberal Democrats, 51% to 60%; Labour, 51% to 57%).
Why is the public satisfied or dissatisfied with the NHS?
We know that public views about the NHS are driven by a range of factors, and that the precise reasons for changes in public satisfaction over time are difficult to pin down (Robertson, 2019). However, since 2015 we have included questions that explore what lies behind the overall levels of satisfaction and dissatisfaction with the NHS reported in the survey by asking respondents to pick up to three reasons for the answer they gave to the overall satisfaction question.1
As Figure 5 shows, more than two-thirds (68%) said they were satisfied because of the quality of care, while six out of 10 said it was because the NHS is free at the point of use. Almost half said they were satisfied because of the range of services available (49%) and the attitudes and behaviour of NHS staff (43%). For just over a quarter (26%), they were satisfied with how long they had to wait for a GP or hospital appointment.
While there have been some small but statistically insignificant changes between 2018 and 2019, the top five reasons given have not changed over the last five years (Figure 6).
In 2019, the top three reasons given by respondents who were dissatisfied with the NHS related to staffing, access and resourcing (Figure 7). Almost two- thirds of people (62%) said they were dissatisfied because of staff shortages, while over half cited long waiting times (57%). Around half said they were dissatisfied due to a lack of government funding (49%). A quarter (26%) identified waste of money as a reason, while one in five (21%) cited the quality of care.
For the past three years of the survey, the top three reasons for dissatisfaction with the NHS have not changed: staff shortages, length of waiting times and money being wasted in the NHS (Figure 8). Looking at how reasons for dissatisfaction have changed, concerns about staff shortages have overtaken dissatisfaction due to waiting times as the main reason for dissatisfaction, with a statistically significant increase of 10 percentage points to 62% in 2019.
The proportion of respondents citing a lack of funding as a reason for dissatisfaction has remained relatively constant over the last three years.
As in previous surveys, very few people said their satisfaction or dissatisfaction was affected by stories in the media – despite widespread media coverage about pressures on the service including staff shortages. However, previous studies have identified links between public levels of satisfaction with the NHS and media coverage (Judge and Solomon, 1993; Judge and others, 1992). It may be that media stories have an indirect impact on underlying attitudes, which is not immediately obvious to the respondent.
Box 1: The NHS and social care in the media during 2019
Before the survey period
In January 2019, NHS England launched its Long Term Plan for the health service with newspaper headlines claiming the NHS was on a ‘mission to save 500,000 more lives'. By February, the health service was midway through another difficult winter and journalists reported plans from NHS England to scrap key A&E targets and replace them with new ones. With an imminent exit from the EU on the cards, in March attention turned to whether Britain would be stockpiling vital medicines ahead of a no-deal Brexit.
Many major NHS targets for hospital treatment were continuously breached last year, but April saw new statistics showing the number of patients who had to wait more than 12 hours for admission to hospital via A&E departments tripling in a year. At a NATO Summit in June, US President Donald Trump declared that the NHS would be ‘on the table’ during any US–UK trade talks. The backlash resulted in a U-turn by the President the following day. There were also headlines throughout the year highlighting staff shortages in the NHS, with reports of increasing levels of staff vacancies.
Survey period
Fieldwork for the current BSA survey was carried out between July and October 2019 during a period of significant political developments. Boris Johnson became Prime Minister in July, after which there was a flurry of announcements on the NHS and social care. He used his first speech outside Downing Street to pledge to fix social care ‘once and for all’ and promised money to upgrade hospitals. He also said that people were waiting too long for GP appointments.
The funding announcements over the ensuing months included money for capital funding, nurse training budgets and social care. The government announcement of plans to build ‘40 new hospitals’ resulted in some debate about how many there would be in reality.
In October 2019 a general election was called. As ever, the NHS played a key role, with debates focused on staffing, trade deals and privatisation.
How satisfied is the British public with different NHS and social care services?
In addition to asking about overall satisfaction with the NHS, the BSA survey asks the public how satisfied or dissatisfied they are with different NHS services: general practice, dentistry, inpatient and outpatient services. Questions were added in 1999 for A&E services, and in 2005 for local authority social care services.
GP services
Over the last few years satisfaction with GP services has been falling, although satisfaction has remained relatively high compared to most other services. In 2016, 72% of those surveyed said they were either ‘very’ or ‘quite’ satisfied with GP services. This dropped to 63% in 2018 – the lowest level recorded since the survey began. This trend was reversed in 2019 with a significant increase in satisfaction of 5 percentage points, bringing it to 68% (Figure 9).
Levels of dissatisfaction have also fallen. In 2018 almost a quarter (24%) of respondents said they were dissatisfied with GP services. This fell to one in five (20%) in 2019.
Despite the significant change in 2019, it should be noted that this level of satisfaction is still one of the three lowest figures recorded since the survey began in 1983, and some way below the recent high in 2009, when 80% said they were satisfied with GP services.
The GP Patient Survey – which hears from almost 800,000 people every year – has seen similar declines over the last few years, particularly concerning overall experience and most notably patients’ overall experience of making an appointment.
Dentistry
Over the last decade, changes in satisfaction with NHS dentistry services have followed a very different pattern to that for GP services (Figure 9), with satisfaction rising from a low of around 42% in the early-to-mid 2000s to a level similar to the NHS as a whole in 2019.
Inpatient and outpatient services
The survey also asks about satisfaction with inpatient and outpatient services (Figure 10). Satisfaction in 2019 with inpatient services remained constant at 64% – its highest level since 1993. Dissatisfaction with inpatient services remained at 9%.
Satisfaction with outpatient services remained consistently high at 71% in 2019 – the highest level since the survey began in 1983. Similarly, dissatisfaction has remained at the same level as 2018, at 11%.
Accident and emergency services
Satisfaction with A&E services was at 54% in 2019 and has not changed significantly since 2018. Levels have remained at similar levels since 2015 and are lower than other NHS services.
Social care
Satisfaction with social care services provided by local authorities was 29% in 2019 (Figure 11), and dissatisfaction with social care services was 37%. Both results are consistent with the previous year.
It is noteworthy that, when asked about their satisfaction with social care, 35% of respondents either said they ‘don’t know’ or that they were ‘neither satisfied nor dissatisfied’ – a much higher proportion than chose these responses for NHS services (Figure 12).2
When reviewing quantitative survey questions about social care, it is important to note that public understanding of social care is relatively limited compared to people’s understanding of NHS services (Bottery and others, 2018). Some caution should therefore be applied when interpreting the data: the high numbers of respondents stating they ‘don’t know’ (8%) or saying they are ‘neither satisfied nor dissatisfied’ (27%) when asked about their satisfaction with social care reflects both this lack of understanding and the fact that only 14% of those surveyed had had some contact with social care services in the last year (compared to 87% who had seen a GP and 54% who had seen a dentist, for example).
Does having contact with a service make people more or less satisfied?
Findings from previous BSA surveys and other studies of satisfaction with the NHS and social care (Robertson and others, 2019; Ipsos MORI, 2017) show that use of, or contact with, services – whether through personal experience or that of friends or family – is one of the factors that influences respondents’ satisfaction ratings. If respondents have had contact with a service they will be taking their experience into account when asked to say how satisfied or otherwise they are with that service. People who have not used a particular service will rely more on indirect information, such as media reports or anecdotal evidence from friends and relations. But to what extent does recent use or contact with a service make people more or less satisfied?
In previous years, the BSA survey only asked whether people had used inpatient or outpatient services recently. For the 2019 survey, we added questions to help us understand the relationship between satisfaction and use of other services, including GPs and social care.
For the 2019 survey we introduced new questions asking whether respondents had used or had contact with a wide range of health and care services in the last 12 months, either personally or on behalf of someone else (see Figure 13 notes).
Figure 13 shows the percentage of respondents who had had contact with each of the respective services. Unsurprisingly, NHS GPs are the service the vast majority (87%) of respondents reported having contact with, while social care is the service with the lowest reported contact levels (14%). Overall, only 4.5% of respondents reported having no contact with any of the services.
How does recent contact with a service affect satisfaction with that service?
Overall, as shown in Figure 14, those who have used or had contact with a service tend to be more satisfied than non-users across all services. This is particularly the case for dentistry, inpatient and outpatient services, where the difference in satisfaction between users and non-users is statistically significant. The highest levels of satisfaction among users were for outpatients (78%), dentistry (77%) and inpatient services (76%).
The difference in satisfaction between those who had had contact and those who had not had any contact (net satisfaction) was greatest for dentistry, with a 37% difference.
So, use of or contact with services suggests that people who have had contact are likely to be more satisfied than people who have not had contact. However, as Figure 15 shows, it is also true that apart from dentistry, those who had contact with services were also more likely to be dissatisfied across all the services. In particular, it is notable that dissatisfaction with social care services was high for both those with and those without recent contact compared to other health services.
However, the difference in dissatisfaction between users and non-users was only statistically significant for dentistry and A&E services.
The dissatisfaction with dentistry is interesting, since it is the only service where dissatisfaction among those who had not had contact in the last 12 months was higher than those who had had contact. This may reflect the difficulties some people experience in accessing an NHS dentist, with the higher levels of dissatisfaction among non-users being a direct result of an inability to access a dentist. Previous research has found that around a quarter of adults do not use dentistry services because they are unable to find an NHS dentist (Appleby and others, 2017).
So, how can it be true that those who have had contact with a service can be both more satisfied and more dissatisfied?
The answer probably lies in the fact that those who have used a service tend to have an opinion on satisfaction, one way or the other, while those who have not tend to have a more neutral position (or say they ‘don’t know’). For example, when asked about satisfaction with inpatient services, 34% of those who had had no contact answered ‘neither satisfied nor dissatisfied’ or ‘don’t know’ – as opposed to 12% of those who had had contact. For dentistry, 41% of those who had had no contact answered ‘neither satisfied nor dissatisfied’ or ‘don’t know’, whereas the equivalent figure for those who had had contact was 11%.
Attitudes to NHS spending and sources of funding
Since 2014, the BSA survey has asked the public about their views on whether the NHS was facing a funding problem, and if so, whether it was minor, moderate or severe (or whether it did not have a funding problem). Between 2014 and 2017 the proportion saying that the NHS faced a major or severe problem rose from 72% to 86%. But this fell in 2018 to 83% and now, in the latest survey, it has again fallen, to 80%. Although this latest drop is not statistically significant, the reduction over the two years from 2017 is significant (Figure 16).
While concern about funding remains very high, the reduction of around 6 percentage points over the last two years coincides with the announcement of increased funding for the NHS by the then Prime Minister Theresa May in the summer of 2018 (then since re-announced during 2019).
This drop in the proportion of respondents expressing worries about funding is also reflected in responses to a related question asking, if the NHS needed more money, how this should be raised for the NHS – a question which has been asked each year since 2014.
Of the six options respondents are given, the proportion saying the NHS should not be given extra money and that it should live within its budget has continued to increase, from 15% in 2017, to 17% in 2018 and now to 20% in 2019 (Figure 17). At the same time, while remaining the most popular choice, the proportion saying extra funding could come from an earmarked tax for the NHS has dropped significantly, from 34% in 2018 to 29% in 2019.
Overall, paying more through some form of tax (either a separate tax that goes directly to the NHS or through current taxes) remains the view of the majority (54%) of those surveyed, with other options such as a £10 charge for GP or A&E visits (11%), paying for non-medical costs in hospital (9%) or ending exemptions for patient charges such as prescriptions (3%) remaining least favoured.
Views about past and future general standards of care in the NHS
As Figure 18 shows, between 2008 and 2011, those surveyed who said that standards of care were getting better over the last five years outweighed those saying it was getting worse. However, between 2014 and 2017 this reversed. In 2017, only 17% said standards had got better and 45% said it had for worse (a net low of –28%).
However, the proportion thinking the NHS had got better started to increase in 2018 (to 20%), and those thinking it had got worse reduced (to 39%). The latest results again show a slight increase in those thinking standards had got better (21%), and a 3 percentage point fall in those thinking they had got worse (to 36%). The changes over the two years from 2017 to 2019 were statistically significant, but it remains the case that the net view remains negative (–15%).
When asked a similar question about standards of care – but over the next five years – similar increases in optimism seem to be emerging over the last two surveys (Figure 19). In 2017, 56% thought standards would get worse over the next five years, and just 20% thought they would get better (a net figure of –36%, the lowest since this question was first asked in 2011).
However, in 2018 this view improved, with a 5 percentage point rise in those thinking things would get better and a similar percentage reduction in those thinking things would get worse. The latest results for 2019 show a rise in the former to 29% and a reduction in the latter to 42%. Nevertheless, the net view remains negative (–14%).
Overall, while people still seem fairly pessimistic both about past and future standards of care, there is evidence of a positive shift in opinion.
Conclusion
The COVID-19 outbreak will put the NHS and social care services under extraordinary strain over the coming months, and the impact of dealing with this crisis is likely to continue well beyond the point where the virus is under control. COVID-19 and the response to it is changing the NHS and wider society in ways no one foresaw, and it will undoubtedly have a longer-term impact on public attitudes to both the NHS and social care. As yet, this impact is of course unknown. It may be that images and experiences of health and care staff working to their utmost capacity in the current crisis will only reinforce the public’s long-term support for the principles of the NHS and their willingness to pay for it. Just possibly, it could also begin to extend some of that concern to social care as well.
In light of the above, what does the 2019 British Social Attitudes survey tell us about the view of the public in the period before the COVID-19 outbreak?
Given the well-publicised and continued failings of the NHS to meet headline targets such as waiting times for elective, emergency and cancer treatments in the period leading up to the survey (Morris and Davies, 2020), it may seem paradoxical that the latest results for overall satisfaction with the NHS show a significant rise – from 53% to 60%. But we know from previous surveys not to assume that satisfaction reflects views about the current performance of the NHS. How the British public responds reflects a more complicated set of factors – some based on personal experience, some on politics and others subject to beliefs about the nature of the NHS as an institution.
Apart from the NHS increasingly making headlines for failing to hit targets, the other piece of news (aside from Brexit) prior to and during the period covered by this research was a series of announcements of higher funding for the NHS. Breaking with a decade of austerity, in the summer of 2018 – the year of the NHS’s 70th anniversary – the then Prime Minister Theresa May announced a new five-year settlement for the NHS that would see its funding increase by £33.9 billion in cash terms by 2023/24 – equivalent to a real increase of £20.5 billion (GOV.UK, 2018). This announcement was reiterated in the 2018 Budget in October of that year (HM Treasury, 2018), then again in August 2019 by the new Prime Minister Boris Johnson (GOV.UK, 2019).
These announcements (and associated promises of more staff, shorter waits for GPs, etc) could be key in explaining the upturn in satisfaction with the NHS and some of its services. Improving views since 2017 about future standards of care in the NHS and its funding needs support an interpretation that the public have understood (and believed) that NHS funding is increasing and that this in turn has fed through to an increased optimism about the future of the service and the difference the money could make.
However, the satisfaction rating for social care remains stubbornly low (at 29%), and some way below that of any of the NHS services. Moreover, users of social care were more dissatisfied than users of any other service, with almost one in two (47%) saying they were dissatisfied. This and many other governments have promised to ‘fix’ social care, but so far these have remained only promises, and there has been no actual reform of an increasingly challenged sector.
While government announcements of extra money for the NHS may have shifted public satisfaction with the NHS, this is only the first step. It is the way extra funds are used to deliver falling waiting times and better care in the medium term that will ensure growing satisfaction with the NHS. This challenge should not be underestimated. There is now rising concern from the public about staff shortages and recognition that this is the biggest problem facing the NHS, so delivering on commitments to increase nurses, GPs and other staff will be key to further improving overall satisfaction.
Footnotes
- The lists of reasons were originally developed with the public by using answers to an open-ended question about why respondents were either satisfied or dissatisfied.
- (Back to text)
- The survey question about social care services has been asked since 2005, although the first two years’ data is based on a question with slightly different wording, which does not mention local authorities in its definition of social care (see notes under Figure 10 for more detail on question wording). (Back to text)
Partners