Professor Tim Briggs grabbed the headlines recently with his assertion that the NHS does not deserve more money until it puts “its house in order”.
He argued that the NHS could save hundreds of millions, if not billions, a year if the best and most efficient practices were applied across the country, a conclusion he reached on the back of his work on the Getting it Right First Time (GIRFT) programme, and fuelled by the findings from their recent work on general surgery.
Like others, I am sceptical that reducing “unwarranted variation” will deliver all the savings anticipated, and certainly not without the necessary support for change management at a local level. And the focus on the potential savings from reducing unwarranted variation misses the much more important gains – the potential improvements in patient outcomes.
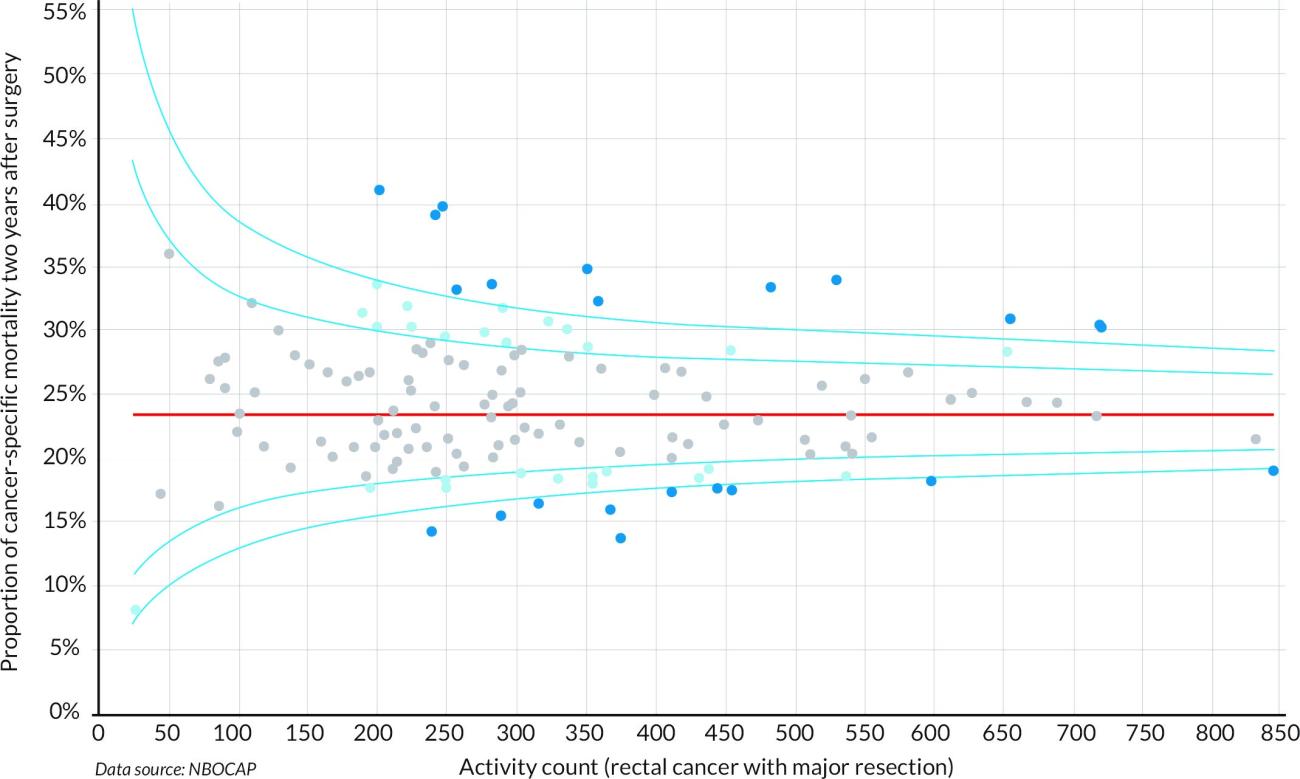
The GIRFT work on general surgery found disturbing levels of variation in clinical outcomes. The 90-day mortality following major resection for colorectal cancer, for example, varies from zero to over 10 per cent, with wide variation between centres undertaking similar volumes of care (see chart below).
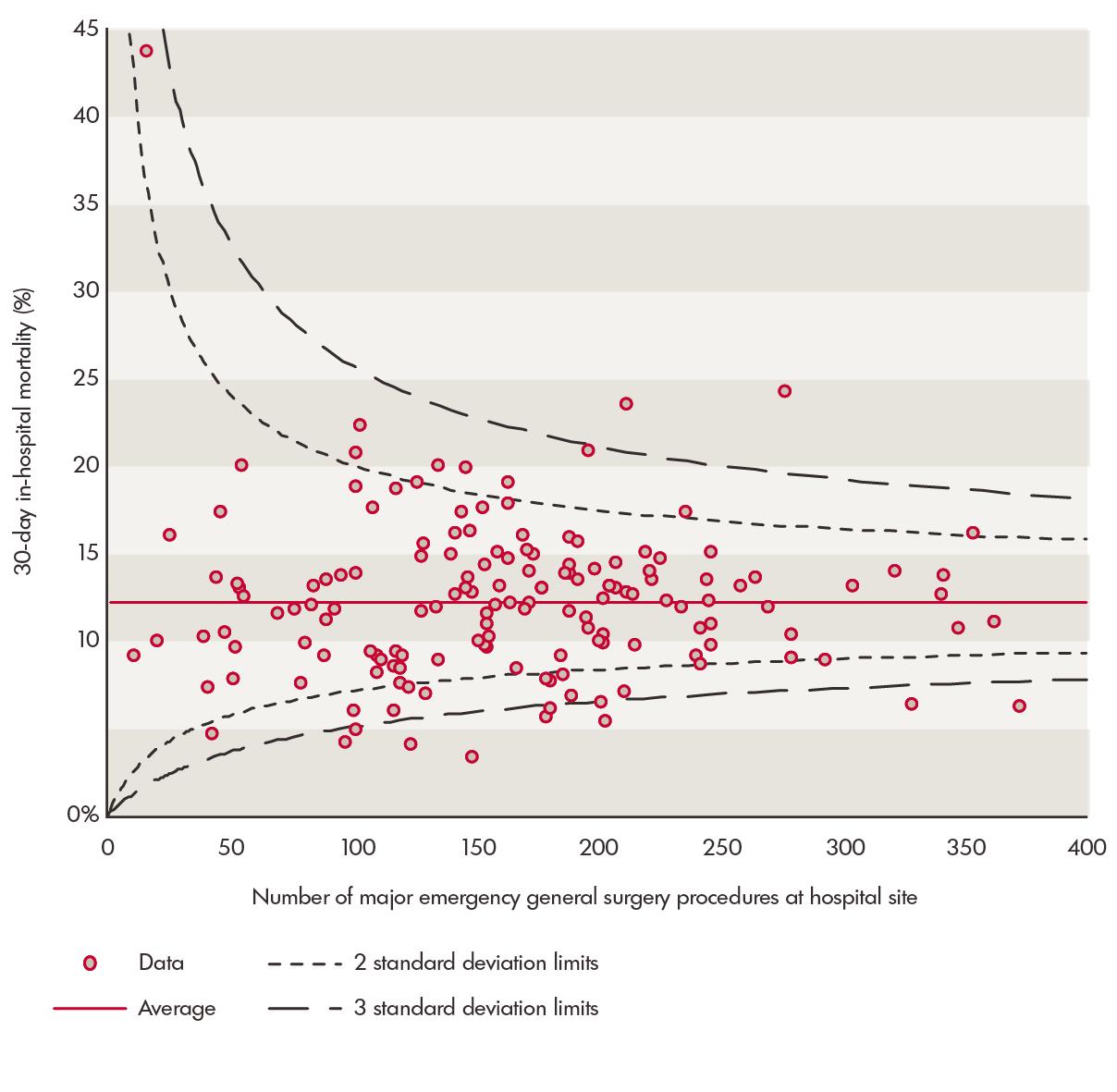
The findings echo those of our recent report on emergency general surgery, where we found that crude rates of 30-day in-hospital mortality for people undergoing a major emergency general surgical procedure varied between around 5 per cent to 25 per cent. One outlier hospital actually had a rate of over 40 per cent.
The variation in outcomes is mirrored by even wider variations in treatment regimes. The use of pre-operative radiotherapy for patients with rectal cancer varies between zero and 80 per cent; the use of chemoradiotherapy as the primary treatment modality for oesophegeal squamous cell carcinoma varies between 30 and 60 per cent; the use of minimally invasive surgical techniques for colorectal cancer surgery between 10 and 100 per cent. These choices will have profound effects on speed of recovery and outcomes.
The variation raises serious issues about variations in individual practice, poor awareness of variation, and a lack of guidance at a national level.
One of the strengths of the GIRFT programme is the direct face-to-face engagement with individual clinicians who are too often rather unaware of other treatment approaches, even in neighbouring hospitals.
The level of variation has led the GIRFT programme to question the current level of autonomy currently experienced by NHS surgeons, and recommend that England considers models such as those in the US and Germany where hospitals appoint specialty leads to set standards and control local ways of working.
It also suggests that our current approach to medical revalidation needs rethinking. It currently relies on a process of local professional appraisal to assess whether doctors are “up to date and fit to practise in their chosen field and able to provide a good level of care”, but does not intervene proactively to ensure that the continuing professional development (CPD) opportunities chosen by the surgeon are the most relevant.
GIRFT has shone a light on high levels of unwarranted variation in clinical practice and outcomes. A light that others, such as the National Confidential Enquiry into Patient Outcome and Death (NCEPOD), NHS Right Care and the National Clinical Audit Programmes have shone before, and over many years.
Yet as GIRFT has shown, the NHS still needs to put its house in order. Engagement by clinicians with up-to-date evidence on variations in outcomes is one important step. More fundamentally, the current levels of clinical autonomy need to be challenged. Clinical autonomy comes at cost, most importantly to patient experience and outcomes.
Suggested citation
Imison, C (2017) "Putting the NHS house in order: putting quality before money" Nuffield Trust comment www.nuffieldtrust.org.uk/news-item/putting-the-nhs-house-in-order-putting-quality-before-money