Debate about the NHS has intensified as the election draws closer, and many of the same myths are being recycled by politicians of all persuasions. Here we examine 10 of the most commonly heard untruths you might hear about our health service in the run up to the election.
1. “There’s been massive privatisation under this government”
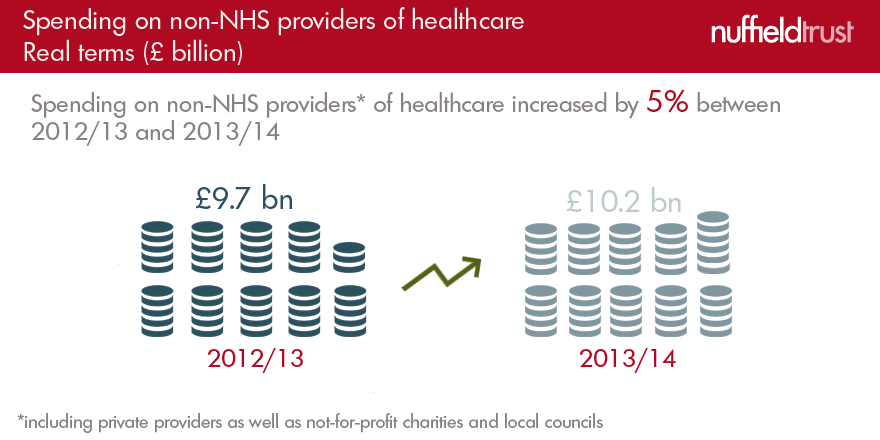
In the most recent figures, £10.2 billion was being spent on non-NHS providers (which includes private providers as well as not-for-profit charities and local councils). That’s an increase of five per cent on the year before. But given that the NHS budget rose by three per cent across the board, the proportion didn’t change much.
Overall, only 5.9 per cent of health service spending in 2013/14 went to private companies aiming to make a profit. The vast majority of the NHS budget, especially for hospital care, still goes to NHS trusts in the public sector.
2. “There hasn’t been any privatisation under this government”
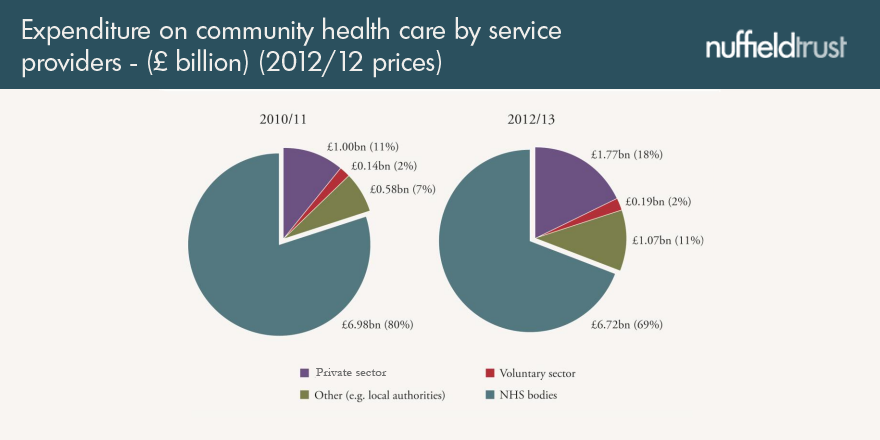
On the other hand, it’s not as if privatisation in the English NHS has been made up. Our analysis shows that in community health care (district nurses, physiotherapists, and so on) and in mental health care, the private sector really did take over a lot of work quite quickly at the start of this parliament, and now accounts for a large proportion of NHS-funded work.
In community health care, the amount of money going to for-profit companies rose by 76 per cent in just two years; if you were counting the ££s, that’s an extra £770 million. It also rose by 18 per cent in hospital care, although the overall proportion is still small at just 3.6 per cent of all the money spent on this area
3. “We need to get rid of all those bureaucrats and managers to save the NHS”
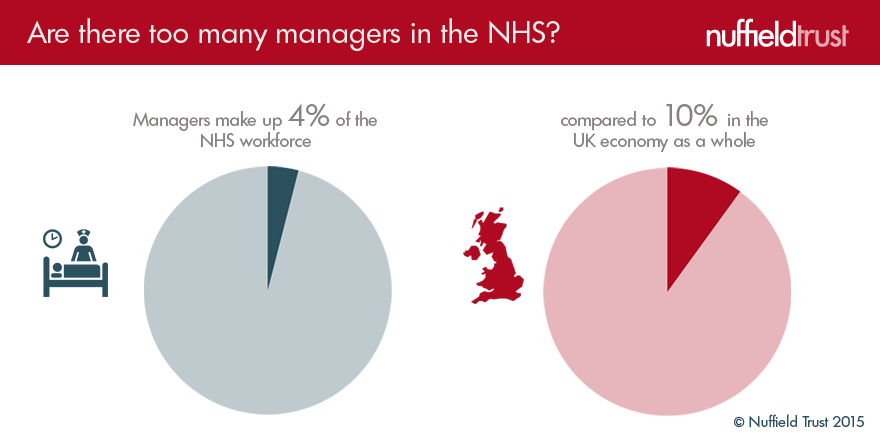
Voters and doctors alike enjoy a good gripe about the NHS being held back by bureaucrats. But actually, only four per cent of the NHS workforce are managers, compared to 10 per cent in the UK economy as a whole. The scope for saving any more money is pretty limited.
Instead of focusing on the number of bureaucrats, it might be better to look at the amount of bureaucracy. There’s a lot – some of it inevitable, some of it less so. Running an organisation the size of the NHS means there will always be unavoidable complicated management to do, but policies like targets create extra paperwork.
Without a particularly large number of full-time managers, NHS doctors and nurses actually end up taking on a lot of this burden.
4. “Immigrants are crippling the NHS”
Rhetoric popularised by certain politicians, and certain newspapers, might have you believe our health service is threatening to buckle under the strain of foreign patients. In fact there is not much hard evidence behind all this.
Aside from the fact that immigrants make up at least 11 per cent of the NHS workforce, research from 2011 also suggests that probable immigrants actually used hospital care at around half the rate of English-born people of the same age and sex.
The study of hospital use agrees with other work that points to something called the “healthy migrant effect”. People who are seriously ill tend not to want to up sticks and move to another country looking for work. As a result migrants are generally healthier than average – and so less likely to turn up in hospital.
5. “We’ve set aside the money the NHS needs”
In this age of rising population, new miracle treatments and spreading waistlines, NHS England says it needs at least £8 billion in extra annual funding by 2020.
This would keep spending per person flat when you “adjust for age” - taking into account that an over-65 or a baby has higher health needs than other groups. Along with massive efficiency savings, that might be enough to keep standards up – bearing in mind that the NHS is already given less money than health services in France and Germany.
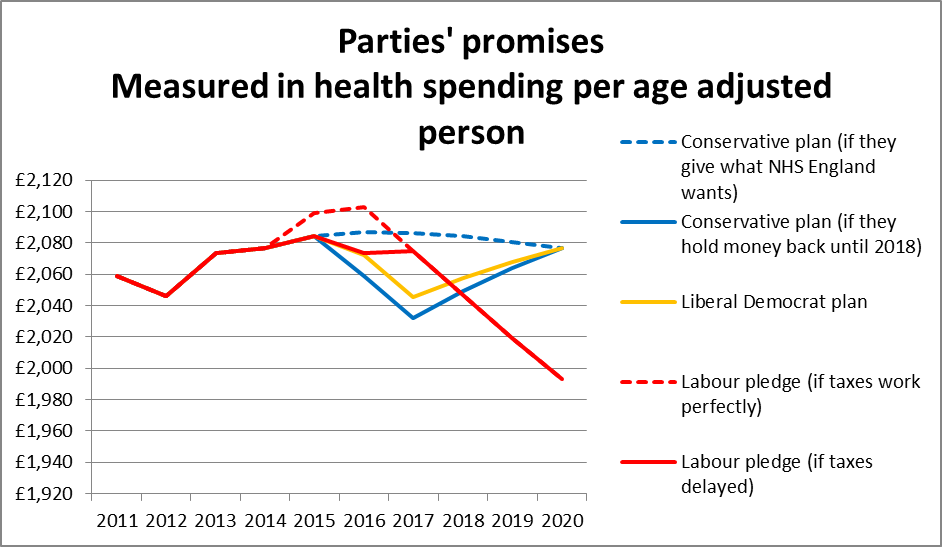
The Liberal Democrats and the Conservatives have both pledged to pay the £8 billion in full for 2020 . The graph above shows these spending plans per age-adjusted person.
You’ll notice that the Lib Dems are actually not promising as much as NHS England wanted in the early years of the parliament: they would let cash per age adjusted person fall by about £40 in the first two years, as they go for cutting the deficit first.
The Conservatives have given the impression they’ll foot the bill in full, keeping funding per person up… but left the wriggle room to do even less than their Coalition partners, chopping £50 per age adjusted person if they delay the funding boost to the end of the parliament.
Labour has promised a smaller funding increase of £2.5 billion after a few months in government, when the cash from its Mansion Tax comes through.
But this will be quickly absorbed by rising numbers of people, and population aging. Without more money, the amount available per person will fall sharply over the rest of the parliament
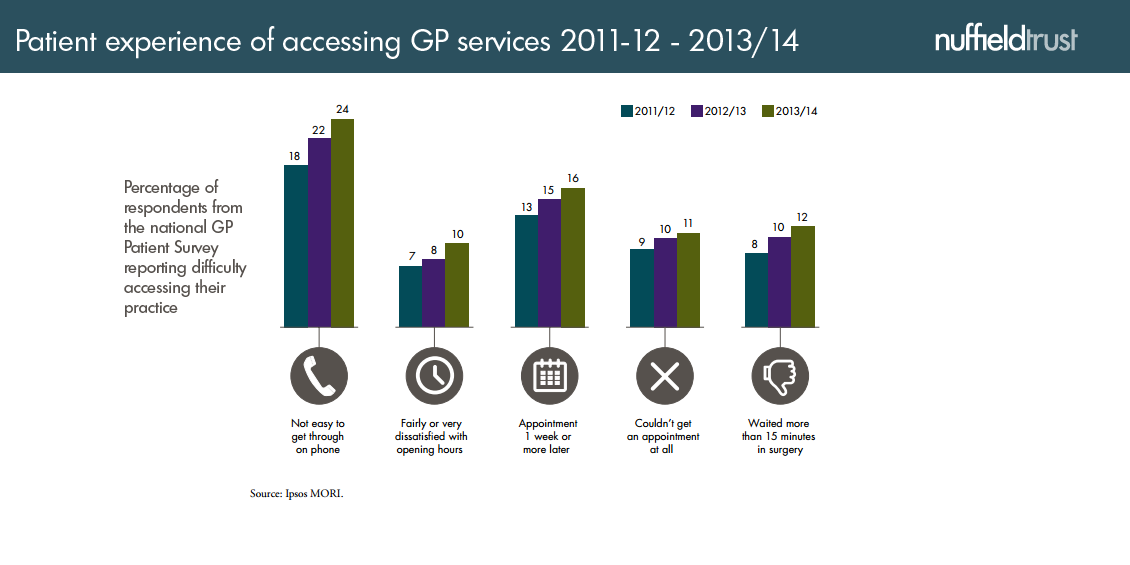
6. “GPs are in meltdown!”
There’s no doubt that, like every bit of the NHS today, general practice is under pressure and as a result, getting an appointment has become a bit more difficult. Statistics are hard to come by, but our recent work showed that the number of patient consultations in a sample of practices had risen by a tenth since 2010 . Meanwhile, the amount of money being spent on them has shrunk.
But although this is a real issue, there’s no need to get carried away. Surveys suggest that the vast majority of people still manage to get appointments, within two days if they want them, and most of them find the timing convenient. We’re not seeing any signs that standards of patient care are slipping.
7. “We have a new target that will guarantee better patient care”
Targets have their place. They can offer a tangible way to measure improvement and performance in specific parts of the NHS, which is hard to do objectively otherwise. And there have been some successes from implementing them. Targets applied by New Labour on areas like waiting times and smoking quit rates in the early noughties were generally achieved (with a bit of help from Blair and Brown’s bumper budget increases).
But the success of those targets can be attributed to large scale pressure issued from the centre, which can create an unhelpful blame culture at the expense of quality.
Holding systems to account is important, but there is a risk that popular-sounding, easily counted targets miss some things that matter for patients. And as more and more hospitals miss their targets, it’s becoming clear that they alone are not enough to drive improvements.
8. “The Welsh NHS is way behind everyone else”
While it’s true that in some areas the Welsh NHS are lagging, in others they’re actually doing slightly better than in England, (like referral waiting times for cancer treatment).
And to be fair to the Welsh government, Westminster rules mean they probably get less money to start with than an equally deprived region of England would receive. They’ve also chosen to protect local authority (and therefore social care) budgets over health, where England has taken the opposite approach (although this is due to change).
Plus, contrary to popular belief, Welsh patients really aren’t inundating English hospitals. There has been no huge increase in the treatment of Welsh patients in English hospitals. In fact, the number has fallen slightly since 2009/10.
9. “The Welsh NHS is fine - nothing to see here”
However, that’s not to say there isn’t cause for concern in Wales.
In many cases, their performance has deteriorated compared to England. Performance on waiting times for planned hospital admissions, decisions in A&E, and ambulances arriving for life-threatening incidents have all fallen significantly. Many Welsh targets have not been met for years.
And while English hospitals are also struggling to meet targets, their performance is generally higher than in Wales. In February 2014, just 51 per cent of Welsh ambulances responded to life threatening calls within eight minutes, compared to 68 per cent in England.
But it’s important to remember that comparing health systems is tricky, and must take into account differing populations, budgets, commissioning decisions and other factors. Which leads us onto our final myth…
10. “Our NHS is better than theirs!”
It’s common to hear unfavourable comparisons between the four health systems of the UK, which have been devolved since the late nineties.
But while it might be tempting to get competitive, there’s little cause for any of us to be too smug about any one country’s performance.
In fact, research has found few signs that one country is drastically outperforming the others – all four countries are keeping pace in measures from life expectancy to stroke care quality.
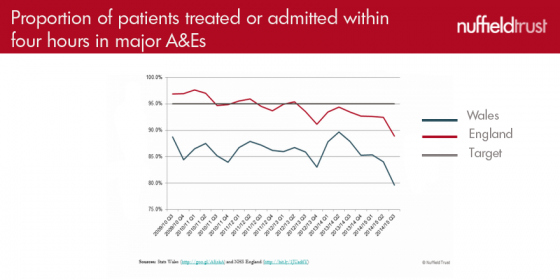
And where performance does differ, it’s not necessarily quite as simple as one country winning. For example, England is the only country ever to reach 95 per cent target of A&E four hour waiting time. But this could be attributed to a knuckle-down approach from English politicians and their, ahem, rigorous methods of upholding the target.
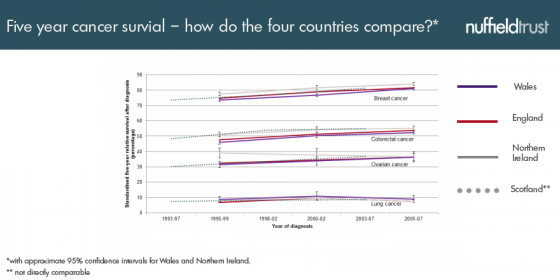
It’s also hard to directly compare data – for example, the way that cancer survival is measured in Scotland compared to the other nations is different which makes it difficult to get a clear picture. With such limited and clouded data; there’s really no country that holds the bragging rights.
A version of this blog was previously posted on Buzzfeed Community.