The government intended that the NHS Test and Trace service in England would “play a vital role” in controlling the pandemic. The subsequent endeavour has come at a huge cost – now expected to be some £22 billion this financial year, equivalent to around £950 per household.
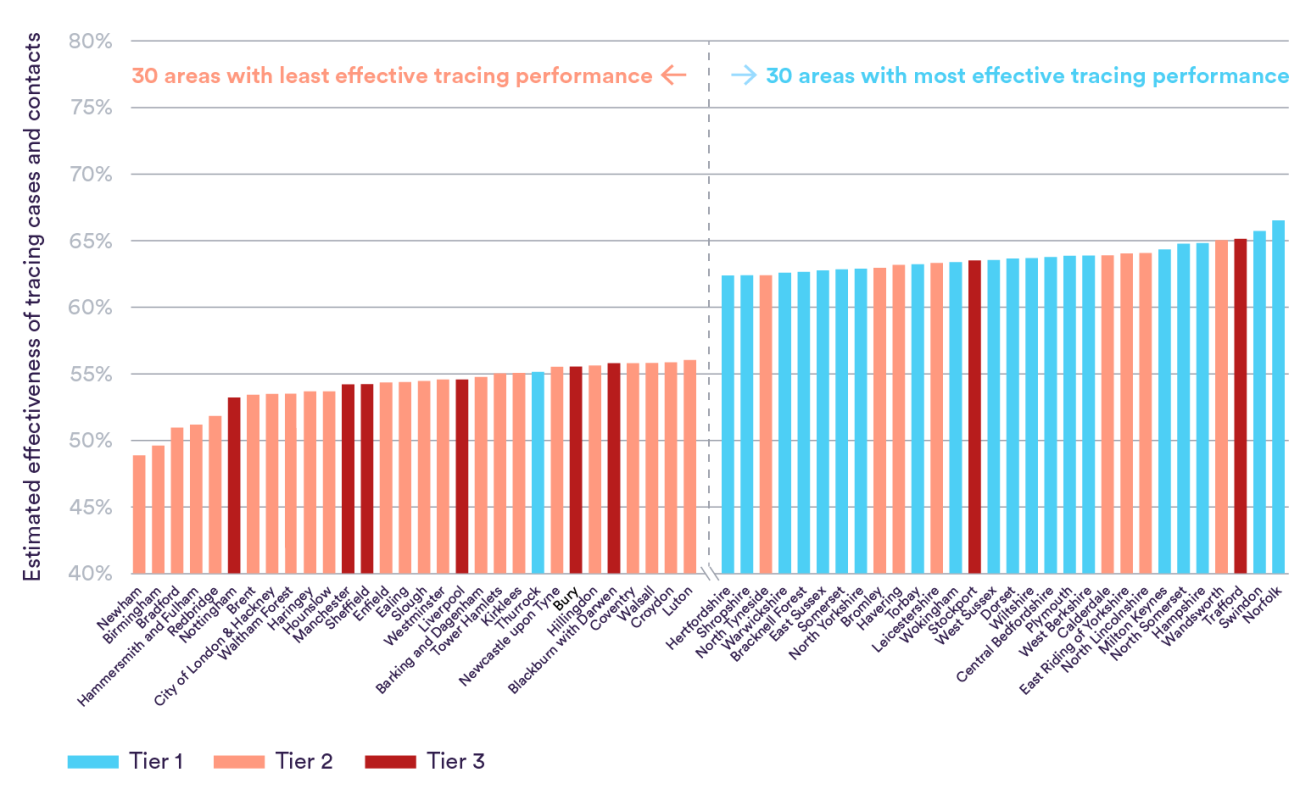
In reality, as we have highlighted previously, the system for identifying positive cases and notifying them and their recent close contacts to self-isolate has continued to look somewhat leaky. Exploring the data from the introduction of the programme up to now suggests there are significant differences in success at reaching cases and contacts at a local level, ranging from an estimated 49% in Newham to 67% in Norfolk.
As shown in the chart, of the 30 (one-fifth of the total) local authorities with the poorest apparent tracing performance, only one was considered to be at the lowest level of alert (medium; tier 1) before the second nationwide lockdown in November. In contrast, the majority of the 30 local authorities with the best tracing performance were judged to be tier 1.
So, better test and trace equals less severe restrictions? But of course, such simple associations need to be treated with caution. In particular, it is important to note that:
- The characteristics of an area – such as the nature of work and housing which could affect the type of outbreaks occurring – might simultaneously affect both tracing performance and transmission (and therefore the tier in which an area was placed)
- The attribution of different tier levels was based on a number of considerations, not just levels of Covid-19 – although further exploratory analysis also suggests a correlation between tracing performance and proportion of recent tests being positive
- Where rates of Covid-19 have increased, the tracing capacity could be struggling to keep up rather than the inverse: increasing rates being caused by shortcomings in tracing.
However, other research has also suggested that contact tracing performance is associated with the spread of the virus. Recent analysis found that areas particularly affected by the data processing error (which meant nearly 16,000 cases were not immediately referred for tracing) subsequently experienced a sharp increase in infections that the researchers conservatively estimated to be associated with 1,500 subsequent deaths.
Certainly, given the importance of contact tracing, the enormous costs involved, and the particular struggles some areas have had in controlling the spread of the virus, the public deserves a clear and urgent assessment on the cost-effectiveness of the test and trace programme.