An ageing population and increasing numbers of people with complex health problems who receive care from multiple providers means that the need to deliver better care coordination and integration is imperative. However, delivering coordinated, high-quality, cost-effective care is challenging for the NHS.
This research report and summary, by Rebecca Rosen, James Mountford, Geraint Lewis, Richard Lewis, Jenny Shand and Sara Shaw, describes case studies of four international organisations that are working to deliver integrated care. Much of the focus of previous case studies on integrated care has been on organisations that are structurally integrated and have matured over many decades. The aim of this current work was to study organisations that were relatively young in their development of integrated care, and that have similarities to the NHS.
The integrative processes created an apparently inseparable web of activities to align professional behaviour and deliver integrated care
The case studies identify the factors that supported or hindered integration, and examine in detail the organisational methods used to align incentives and coordinate professional practice in order to deliver integrated services.
The four organisations analysed were:
- Community Care North Carolina, US: a government-funded network that aims to improve access and quality levels for Medicaid beneficiaries;
- Greater Rochester Independent Practice Association, US: an independent practice association in upstate New York;
- Regionale HuisartsenZorg Huevelland, the Netherlands: an organisation providing support to GPs to deliver integrated diabetes care;
- North Lanarkshire Health and Care Partnership, Scotland: an NHS and social care partnership.
The experiences of the four organisations suggest strongly the influence of six groups of operational activities (‘integrative processes’) that served to embed coordinated care into daily practice: clinical, organisational, informational, financial, administrative and normative (see Figure 1 below). In addition national policy, regulation and payment systems were found to be important enablers – or inhibitors – of integrated care.
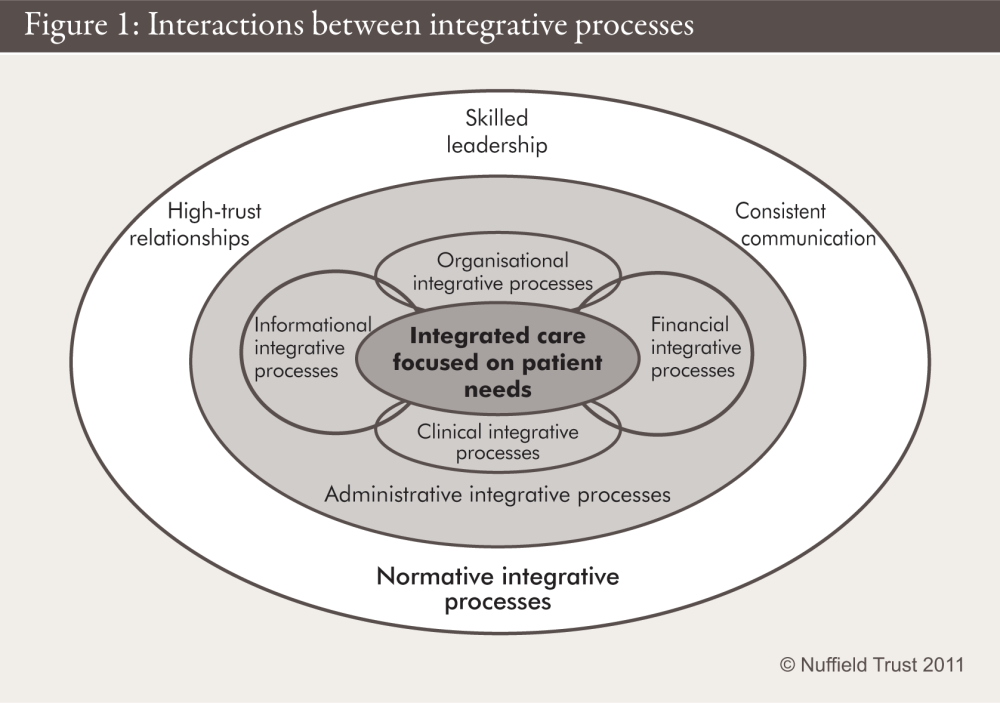
Several proposals in the White Paper Equity and Excellence: Liberating the NHS, the subsequent Health and Social Care Bill and the Government’s response to the report from the NHS Future Forum have the potential to support integration between health services and between health and social care. These case studies offer insights into how policy and regulation could be developed and implemented to support integration between services, and sets out recommendations at both national and local commissioning level for integrating care within the NHS.
Integration in action: four international case studies will be of interest to health and social care policy-makers, senior managers and practitioners, and NHS commissioners, as well as academics and researchers in the fields of health and social policy.
The report forms part of the Nuffield Trust’s extensive programme of work on integrated care, which is examining the potential of new forms of care that are intended to benefit both patients and taxpayers.