Last month, the UK Health Security Agency warned that around one in 10 children starting school were at risk of measles, as vaccination rates dropped to the lowest level for a decade.
A campaign was launched to encourage parents and guardians to ensure children are up to date with the measles, mumps and rubella (MMR) vaccine, highlighting a significant drop in childhood vaccination rates since the start of the pandemic. However, the available data show that the recent decline is in fact part of a longer-term trend. In 2016/17, 87.6% of children had received two doses of the MMR vaccine by their fifth birthday, which decreased to 86.6% in 2020/21.
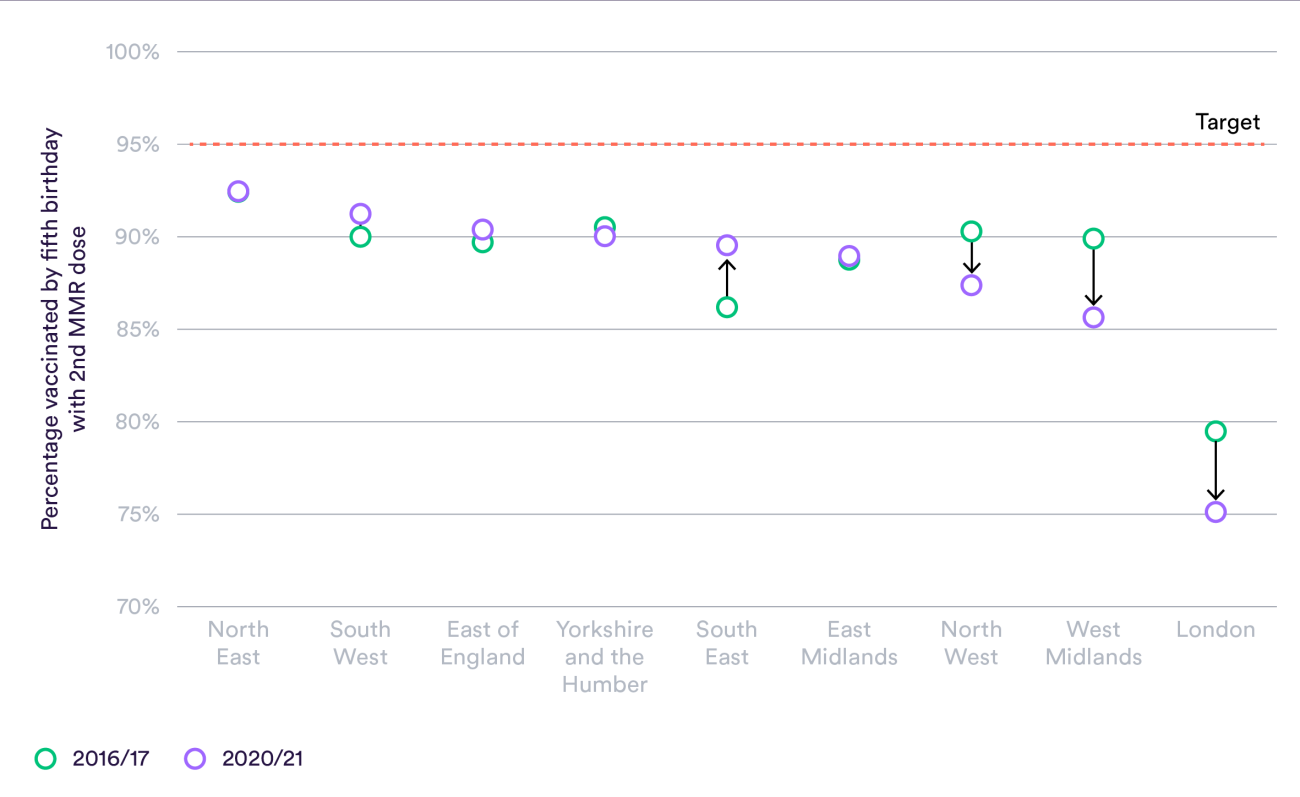
Hidden beneath these figures are considerable differences in MMR vaccine uptake by region in England. Notably, London has the lowest MMR vaccination rate, with one in four children in 2020/21 not receiving their second dose by their fifth birthday. This compares to fewer than one in 10 children in the North East.
None of the regions in England are meeting the World Health Organisation’s 95% target for vaccination coverage – the level needed to achieve and sustain measles elimination. Clusters of outbreaks can occur; in 2019, there were almost 800 confirmed measles cases in England, over half of which were confirmed in London.
The regional differences mimic, to some degree, variation in uptake of other vaccinations such as the Covid-19 vaccine, where rates are also much lower in London. Part of the explanation is that the capital has a more mobile population with many people moving house more frequently, which brings a tendency to not register with a new GP, meaning that vaccination reminders can be missed.
Another reason points towards demographic data, with vaccination uptake lower in some groups such as those from minority ethnic backgrounds. Vaccination hesitancy and misinformation can derail population vaccination campaigns, as we saw in the late 1990s in relation to the MMR vaccine. Recent cuts to public health funding are also likely to be impacting childhood vaccination rates.
Increasing vaccination coverage across the country is vital if we are to prevent measles outbreaks from occurring, which can have serious health consequences. Attention is needed across local areas to assess the barriers to vaccine uptake and the opportunities for improvements.